You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Introduction
The Human Immunodeficiency Virus and Acquired Immune Deficiency Syndrome (HIV and AIDS) are catastrophic illnesses affecting millions of people worldwide. HIV damages and kills the cells of the body's immune system by destroying the body's ability to fight bacterial and viral infections. A person cannot get acquired immune deficiency syndrome (AIDS) without first having HIV. AIDS is the end stage of HIV infection. Without the ability to fight infection, the body is compromised and severe damage occurs, often resulting in hospitalization and death.
The purpose of this course is to provide an overview of HIV and AIDS and to update dental assistants on current trends and treatments of HIV and AIDS. As dental patients will be managing and living longer through the HIV and AIDS illnesses, the dental team must understand the treatment process and disease transmission prevention.
Facts About HIV/AIDS Prevalence
AIDS is the most catastrophic disease in modern history. It has become the world's deadliest infectious disease and is threatening to eliminate up to one-sixth of the world's population. An estimated 33.3 million people worldwide are infected with HIV. In 2009, 2.6 million people were newly infected according to the World Health Organization/UNAIDS. In 2009, there were approximately 1.8 million deaths from AIDS. Current reports estimate more than 2 million people die from AIDS each year; with about 550,000 people dying from HIV-related conditions in the United States. Most people with HIV are living in developing countries, with the highest concentrations on the African continent.
The number of people living with AIDS is increasing, as new and effective drug therapies keep HIV-infected persons healthy longer thus dramatically reducing the death rate. The Centers for Disease Control's (CDC) programs work to improve the treatment, care, and support for persons living with HIV/AIDS. The CDC also works diligently to build capacity and infrastructure to address the HIV/AIDS epidemic in the United States and around the world. From 2006 to 2009 the estimated number of people living with HIV increased 8.2% from 1,061,100 to 1,148,200.
In 2010, a pivotal year, our nation's primary concern was to control and end the HIV epidemic in 2011. U.S. President Obama initiated major policy shifts affecting HIV prevention. There was a lift of the 22-year ban on HIV+ travelers to the U.S.A. and a modification of a twenty year ban on federal funding of needle exchange programs.
When the National HIV/AIDS Strategy (NHAS) was released on July 13, 2010, President Obama charged the U.S. Department of Health and Human Services (HSS), the Departments of Labor, Justice, Housing and Urban Development, Veteran Affairs, and Social Security Administration with lead responsibility for implementing the strategy and gave them 150 days to develop operational plans detailing how they intended to approach this challenge. December 9th marked a milestone in the ongoing efforts to achieve the goals of the NHAS, producing the first comprehensive roadmap for reducing HIV infections in the United States. Five other federal agencies and HHS submitted their NHAS operational plan to the White House.
HIV Incidence Report
This report presents data for diagnoses of HIV infection and AIDS through December 31, 2010 and reported to CDC through June 2011. A supplemental report was made available in 2012.
Incidence is the number of new HIV infections that occur during a given year. The CDC estimates that approximately 50,000 people in the United States are newly infected with HIV each year. In 2010 (the most recent year that data are available), there were an estimated 47,500 new HIV infections. Nearly two thirds of these new infections occurred in gay and bisexual men. Black/African American men and women were also highly affected and were estimated to have an HIV incidence rate that was almost eight times as high as the incidence rate among White people.
The 2010 HIV Surveillance Report Summary
This CDC report includes data reported from 50 states and six U.S.A. dependent areas. For data regarding deaths of people with an HIV+ diagnosis, this was reduced to 46 states and five U.S. dependent as some have not had confidential name-based reporting.
The combined data from 2007 through 2010 reveals:
| • | The annual estimated number and rate of diagnoses of HIV infection remained stable in the 46 states, even though estimated numbers and rates of diagnoses of HIV infection increased in some subgroups and decreased in others. The CDC estimates that there were 47,129 diagnoses of HIV infection in the 46 states in 2010. The estimated rate of diagnoses of HIV infection in the 46 states in 2010 was 16.1 per 100,000 persons. |
| • | The annual estimated number of AIDS diagnoses in the U.S. remained stable, and the rate of annual AIDS diagnoses decreased. CDC estimates there were 33,015 AIDS diagnoses in 2010. The estimated rate of AIDS diagnoses in the U.S.A. the same year was 10.8 per 100,000 persons. |
| • | From the beginning of the epidemic through 2011, there have been 1,155,792 persons diagnosed with AIDS in the U.S. |
| • | The majority of diagnoses of HIV infection were among Blacks/African Americans (46% of all diagnoses of HIV infection), White people (29%), and Hispanic/Latinos (20%). The only racial/ethnic group to have an increase in the rate of HIV diagnoses was American Indian/Alaska Natives. |
| • | By transmission category, the only increase seen in the number of HIV diagnoses was among adult and adolescent males with infection attributed to male-to-male sexual (MSM) contact. |
The 2010 HIV Surveillance Report shows a 10% increase in the number of HIV diagnoses among persons aged 15-19 years and a 33% increase among persons aged 20-24 years. The fact that our young people are bearing a significant burden of the nation's HIV infections has been highlighted in recent CDC publications of HIV incidence and a recent CDC surveillance supplemental report focusing on diagnoses of HIV infection among adolescents and young adults. HIV continues to have a significant effect on young people in the United States, especially young men who have sex with men.
Overall, the CDC's new incidence estimates continue to show that:
| • | Gay and bisexual men remain as the population most heavily affected by HIV in the United States. The CDC estimates MSM represent approximately 2% of the U.S. population, but accounted for more than 50% of all new HIV infections annually from 2006 to 2009. 56% in 2006 (27,000), 58% in 2007 (32,000), 56% in 2008 (26,900) and 61% (29,300) in 2009. |
| • | African Americans and Hispanics/Latinos are the racial/ethnic groups most affected by HIV. African Americans represent approximately 14% of the U.S. population, but accounted for 44% (21,000) of all new HIV infections in 2009. Hispanic/Latinos represent approximately 16% of the total U.S. population but accounted for 20% (9,400) of all new HIV infections in 2009. |
HIV Virology and Immunology
Immunity to a disease is achieved through the presence of antibodies to that disease in a person's system. Antibodies are disease specific, meaning that the antibody for hepatitis B will protect against hepatitis B, but not protect against small pox.
The two types of immunity are active and passive. Active immunity is long-lasting and achieved through infection and recovery (natural immunity) or through the introduction of a vaccination containing the weakened disease whereby stimulating the body's need to recover (vaccine-induced immunity.) Passive immunity is provided when a person is given antibodies to a disease rather than producing them through his or her own immune system. For example, a newborn acquires passive immunity from its mother through the placenta and breast milk. Unfortunately, passive immunity is not long-lasting.
The immune system is a complex network of cells and body organs that work together to defend the body against infection by germs (virus or bacteria) such as HIV. Some of the components included in this system are lymph nodes, bone marrow, blood vessels, the spleen, thymus, and tonsils. Lymphocytes are created within this system. Lymphocytes are a group of infection fighting white blood cells. Lymphocytes that mature in the bone marrow are known as "B" cells and those that move on and mature in the thymus will become "T" cells. Put very simply, the B cells produce specified antibodies and the T cells kill the infectious germs.
As a germ invades a person's system, special white blood cells, called neutrophils, work as antibodies and attach themselves to the germ cells to slow them down. Protector cells, called phagocytes, can begin the process of killing and engulfing them. Phagocytes, in the form of macrophages, come in to clean up and eat the dead cells. After the battle, most of the cells die off while a few T cells survive and become T memory cells. These memory cells remember the battle and are able to fight again should the same invader strike. Thus, the body is said to be immune to that infection.
HIV disguises itself by mutating the outer cell coating. This mutation helps the virus evade antibody detection because the T memory cells only recognize previously encountered invaders. Some of the HIV-infected cells are destroyed when the helper T cells join the battle; however, the HIV attach themselves to the CD4 T cells and the T cells accept the foreign HIV cells as their own. The outer coverings of the two cells fuse, thus the mutation occurs.
HIV is classified as a retrovirus that has a long latency period. HIV invades the body through the bloodstream and uses the immune system against itself. As the macrophages recognize the invader, they attack just as they would for any other foreign substance. Once inside the CD4 helper T cell, HIV uses a reverse transcriptase enzyme to translate its own genetic program ribonucleic acid (RNA) into the T cells' genetic material deoxyribonucleic acid (DNA). Instead of fighting against the infection, the T cell is reprogrammed to either produce more HIV cells or to remain dormant.
In the HIV infection cycle, this is the window period. This is the time period after contracting the infection and until the body has developed enough antibodies for an accurate positive test result. For most people, this can range from two to eight weeks, but in some rare cases it can take up to six months. The HIV infected person is infectious during this time. HIV infection can be detected at this point if initial and confirmation testing is completed.
People infected with HIV eventually develop symptoms that usually last a long time and are often severe. These symptoms include enlarged lymph glands, fever, tiredness, loss of appetite and weight loss, diarrhea, yeast infections of the mouth and vagina, and night sweats.
In the HIV infection cycle, this is considered the incubation period. An HIV infected person may not feel sick or exhibit symptoms of the disease for five to ten years or longer. The disease can still be spread during this period.
As the immune system becomes weaker, the infected person becomes more susceptible to illnesses that normally do not occur in healthy people. These illnesses are called opportunistic infections. The most common opportunistic infections are Pneumocystis jiroveci (formerly known as Pneumocystis Carinii Pneumonia, or PCP), yeast infections of the mouth and esophagus, Kaposi's sarcoma, which is a cancer of certain blood vessels, and human cytomegalovirus which affects the salivary glands, eyes, and sight.
AIDS Lifecycle
Stage 1 - HIV virus is passed from one person to another. The virus travels through the bloodstream to many different places in the body.
Stage 2 - The immune system, which helps the body fight off illness, begins to fight back against the virus.
Stage 3 - The defense is coordinated by the helper T cells. But, the HIV virus attacks the T cells themselves, crippling the body's defenses.
Stage 4 - HIV has a special shape on its surface which, like a piece of a jigsaw puzzle, fits perfectly into a shape on the T cell. This shape is a protein called CD4. HIV uses CD4 to enter the cells it infects. This is why the helper T cell is referred to as a CD4 lymphocyte.
Stage 5 - Once inside a helper T cell, HIV takes over the cell and the virus then replicates. The virus's genetic information (RNA) is transcribed into a form that is identical to the cell's genetic information (DNA). The virus, now in the form of DNA, hides out inside the nucleus of the cell, escaping from the body's defenses.
Stage 6 - After a dormant time, HIV comes out of hiding and begins to reproduce. The DNA is transcribed into many copies of RNA that produces proteins for the new viruses.
Stage 7 - The proteins are cut into usable pieces and packaged with the RNA.
Stage 8 - The new viruses then bud from the cell. Each new virus may then go on to infect and destroy other T cells, weakening the immune system's defense.
Stage 9 - After many T cells are destroyed, the person is said to have AIDS. When an HIV infected person's CD4 count drops to below 200, he or she is said to have AIDS. A healthy person's CD4 count is in the range of 800 to 1200. AIDS also means that the HIV infected person has one or more of the many opportunistic infections. Without a strong immune system, a person with AIDS and an opportunistic infection will eventually succumb to the opportunistic illness.
Oral Manifestations
There are many oral manifestations that can be detected by the dental team. The following lists are often seen in patients with HIV and AIDS. When patients come to the dental office for recare and restorative appointments, the following manifestations may be seen and must be noted in the patient record. If seen for the first time, the patient must be referred for testing and biopsies. Medications to treat these symptoms must be prescribed carefully and best done with the collaboration of the treating physician.
Neoplastic
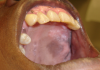
Kaposi's Sarcoma (Figure 1). People with AIDS-associated Kaposi's sarcoma (KS) frequently have oral lesions that visually manifest as red, brown, or purple patches or swellings. The palate is the most common site but lesions also occur on the gingiva, tongue, and oropharynx. KS is usually asymptomatic, but occasionally becomes painful because of ulceration or infection. Bulky gingival lesions that show when the patient smiles or talks may be of concern for cosmetic reasons and may also interfere with oral hygiene. Good oral hygiene and professional prophylaxis is, therefore, important in the management of oral KS. Small, well-localized lesions on the palate or gingiva are usually good candidates for treatment with intralesional injection of vinblastine (a drug used in combination with chemotherapeutics to treat cancers). Surgical removal and the carbon dioxide laser are also sometimes useful in removing such lesions. Small lesions may be treated on several occasions to achieve the best results. Large lesions may respond better to radiation therapy, either in a one-dose treatment or fractionated treatments delivered for ten to twelve days. Some patients experience episodes of mucositis during chemotherapy and xerostomia is sometimes a problem, but usually improve after therapy. Systemic chemotherapy is indicated for widespread or disseminated disease.
Immunoblastic Lymphoma. Oral lesions of AIDS-associated lymphoma may be the first presentation of that tumor. The lesions include firm masses and persistent ulcers. Diagnosis is made from a biopsy, as lesions may mimic other problems. AIDS-associated lymphomas in the mouth are usually large B-cell immunoblastic in type; T-cell lymphomas are also seen, albeit rarely. The oral lesions are treated as part of the overall management.
Bacterial
Periodontal Disease. Although conventional periodontal disease is seen in this population, a much more rapid and severe form occasionally occurs. Formerly called HIV-periodontal disease, this is now known as necrotizing ulcerative periodontitis (NUP). The associated and possible precursor lesion, formerly called HIV-gingivitis, is now known as linear gingival erythema (LGE). LGE may be difficult to distinguish from conventional gingivitis. It appears as a red band along the marginal gingiva and may be associated with complaints of occasional bleeding. NUP is associated with severe pain and bleeding, rapid loss of bone and soft tissue, sometimes leading to exposure and sequestration of bone, mobility, and tooth loss. No unique microorganisms have been identified. Rather, the condition seems to involve an anaerobic periodontal flora similar to that which causes conventional periodontal disease. The role, if any, played by host factors is equally poorly defined. Management of NUP requires care by a dental professional familiar with this condition. Effective treatment depends on the immediate application of local measures, including removal of plaque and necrotic soft tissue by scaling and curettage, and irrigation with agents such as 10% betadine. Where bone is exposed, sequestration may occur, sometimes without tooth loss. Home care is very important. Affected areas need to be irrigated locally with povidone iodine and the mouth rinsed with chlorhexidine. Antibiotics effective against gram-negative flora may be needed in cases of severe disease, but these must be used in conjunction with the local measures described above. Flagyl®, whose active ingredient is metronidazole (one 250-mg tablet taken four times a day) is useful against this condition. Alternatives include clindamycin (one 300-mg tablet taken three times a day) or Augmentin® (one 250-mg tablet taken three times a day).
Tuberculosis. Tuberculosis (TB) is a disease caused by a bacterium called Mycobacterium tuberculosis and usually attacks the lungs. Oral lesions in people with TB are rarely seen. These lesions have been reported as ulcers on the tongue secondary to TB. Mycobacterium avium complex (MAC) is a type of non-tuberculosis mycobacterial infection. Oral lesions are not a common finding in people with MAC, but has been reported to occur as a palatal ulcer and was in fact the first presentation of MAC in that patient.
Viral
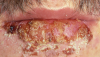
Herpes Simplex (Figure 2). Herpes simplex virus causes both primary and recurrent oral disease. The primary event, herpetic gingivostomatitis, is most common among children and young adults in the general population and it is also seen in young people with HIV infection. Herpetic gingivostomatitis presents as ulcers and vesicles on the gingiva as well as elsewhere on the oral mucosa. The lesions are accompanied by fever and complaints of pain and loss of appetite. Recurrent herpes simplex may involve the lips or the intraoral mucosa. Lip lesions appear as small vesicles that rupture, ulcerate, and then form a crust. Recurrent, intraoral herpes simplex starts as small crops of vesicles on the hard palate or gingiva that rupture to produce small, painful, merging ulcers. Patients with active, puss-filled ulcers should receive only palliative treatment and rescheduled for treatments that can be delayed until the lesions are crusted.
The oral lesions are usually confined to the keratinized mucosa, although lesions may appear on the dorsal surface of the tongue. The buccal mucosa and lateral margin of the tongue are very rarely involved. The lesions may be trivial and self limiting or, occasionally, troublesome, extensive, and persistent. Lesions that are slow to resolve can be treated with acyclovir, 1000 to 1600 mg daily for seven to ten days. Topical acyclovir is not effective in treating intraoral lesions and may not be effective in treating herpes labialis. Occasionally, herpes labialis is resistant to treatment with acyclovir; these lesions may respond to phosphonoformate.
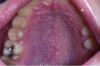
Herpes Zoster (Shingles) (Figure 3). Orofacial herpes zoster, a reactivation of the varicella zoster virus, or chicken pox, produces crops of vesicles along the distribution of one or more branches of the trigeminal nerve. Usually unilateral, the lesions may appear on the skin or intraorally on any mucosal surface. The skin lesions begin as vesicles, then rupture and crust over. The oral lesions are vesicles that rupture to form ulcers. Prodromal complaints may include pain referred to otherwise healthy teeth. Treatment is oral famciclovir (500 mg, every 8 hours for 7 days) or oral acyclovir (800 mg, five times a day for 7 to 10 days) and should be started as soon as possible. Shingles is only contagious to a dental team member who has never had chicken pox.
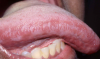
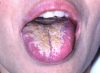
Hairy Leukoplakia (Figure 4). Hairy leukoplakia (HL) is one of the most common HIV-associated oral lesions and is not contagious. It is a nonremovable, white, corrugated or "hairy" lesion seen on the lateral margin of the tongue and occasionally elsewhere on the oral mucosa. AIthough HL occurs in all the risk groups for HIV infection, it is not common in children. Cases of HL have been reported in HIV-negative people in association with immunosuppressive therapy. HL is usually asymptomatic, although patients occasionally complain of its appearance or texture.
Differential diagnosis includes lichen planus and epithelial dysplasia, so biopsy of the lesion may be necessary. The lesion is often secondarily infected by candida, but elimination of that organism with antifungal therapy does not cause the lesion to disappear. HL is caused by the Epstein-Barr virus (EBV), which can be seen during the testing on an electron microscope. As far as can be determined, HL is not a premalignant lesion. HL can be eliminated with acyclovir at doses from 2.5 to 3.0 mg per day for two to three weeks, but the lesion usually recurs when treatment ends. Case reports have described responses to other agents, including ganciclovir, phosphonoformate, Retin A, and podophyllin resin, although, again, the lesion tends to recur within a few months. Although there were initial reports indicating that HL regressed in individuals during AZT therapy, in a larger series, researchers have not found this to be the case.
Cytomegalovirus (CMV) Ulcers. Cytomegalovirus has been found in oral mucosal ulcers, predominantly in patients with known CMV disease. CMV is not highly contagious but has been known to spread to those with weak immune systems through close contact with a person excreting the virus in their saliva or other bodily fluids. In this case, it is important that the dental team employs standard precaution procedures. These ulcers occur on both keratinized and nonkeratinized mucosa, appearing on the gingiva, buccal mucosa, and palate. Oral CMV ulcers may be confused with necrotizing ulcerative periodontitis, lymphoma, and atypical aphthous ulcers. When ganciclovir is used to treat CMV disease, the oral ulcers resolve.
Human Papilloma Virus Lesions. Human Papilloma Virus (HPV) is a common sexually transmitted disease and can lay dormant in the body for many years. As is true in other groups of immuno-suppressed individuals, lesions caused by HPV are common on the skin and mucous membranes of those with HIV infection. In the mouth, these lesions take the form of typical warts, caused by a variety of types of HPV, and focal epithelial hyperplasia (Heck's disease), caused by HPV types 13 and 32. These warts may appear cauliflower-like, spiky, or slightly raised with a flat surface. Application of 5% acetic acid may make them more visible.
Surgical or laser excision is the most effective way to remove HPV warts, but recurrence is common, so removal should probably be reserved for lesions that interfere with function or esthetics. Oral HPV infections are usually uncommon but it is important that the dental team employs standard precaution procedures.
Fungal
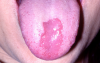
Oral Candidiasis. Like hairy leukoplakia, oral candidiasis is highly prevalent in HIV-infected individuals. Approximately 30% of otherwise asymptomatic gay men have one or both of these lesions, and they are often the first clinical expression of HIV disease. Three presentations of oral candidiasis are seen in association with HIV infection: pseudomembranous candidiasis (thrush), erythematous candidiasis, and angular cheilitis.
Pseudomembranous candidiasis (Figure 5) appears as a creamy, white pseudo membrane that wipes off easily with gauze or tongue blade. It can be found anywhere in the mouth or pharynx. These plaques are not contagious and caused by an imbalance between oral flora and protective mechanisms, often associated with antibiotic use and inhaled steroids.
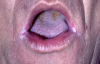
Erythematous candidiasis (Figure 6) presents as flat, subtle, red patches of varying sizes on any mucosal surface, commonly the palate and dorsal surface of the tongue. The tissue is known to be sensitive to the patient. This form of oral candidiasis is predictive of the development of AIDS but also associated with tissue trauma such as denture stomatitis.
Angular cheilitis (Figure 7) involves fissuring and cracking at the commissures (corners) of mouth. Saliva can pool in these cracks causing the patient to lick their lips excessively and be more sensitive to sun exposure. Angular cheilitis is not contagious.
Occasionally, all three types appear in the same individual. The diagnosis of oral candidiasis is usually made from the appearance of the lesions, but a biopsy will confirm the diagnosis.
Oral candidiasis may be treated with either topical or systemic antifungal agents. The choice of medication depends on a variety of factors, including other, concomitant medications, evidence of abnormal liver function, patient preference and compliance, and the sugar content of topical preparations. Topical agents include nystatin oral pastille (lozenge), one or two pastilles dissolved slowly four to five times a day; clotrimazole oral troche (lozenge), 10 mg, one troche dissolved five times a day; and nystatin oral suspension. Nystatin oral suspension has a high sugar content and its relatively short time in contact with the oral mucosa makes it less effective. If used for a long time, the oral topical agents that contain sweetening agents may promote caries, so daily topical fluoride rinses should be used in conjunction with long-term therapy.
Oral candidiasis can be treated systemically with ketoconazole, fluconazole, and itraconazole. Ketoconazole is used as one or two 200-mg tablets taken daily with food. However, since ketoconazole depends on normal levels of gastric acidity for its absorption and many HIV-infected patients have hypochlorhydria, caution should be exercised. Fluconazole is used as one 100-mg tablet taken once daily. Itraconazole is used as two 100-mg capsules taken daily. Oral candidiasis outbreaks often recur and maintenance therapy may be needed.
Angular cheilitis can be treated with topical agents such as nystatin, clotrimazole, and ketoconazole creams or ointments. Some cases of oral candidiasis may be resistant to treatment with fluconazole and to other orally administered systemic and topical agents. Amphotericin B solution has been reported to be helpful in some of these cases. Amphotericin B as an oral solution is prescribed as 0.1 mg/ml; 5 to 10 ml is used to rinse the mouth and is then expectorated, three to four times a day.
Histoplasmosis. Histoplasmosis is frequently seen in people with cancer or AIDS. It has been reported to present rarely as oral ulcers that may be the first presentation or may be part of disseminated disease.
Others
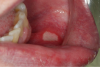
Oral Ulcers. Oral ulcers of several types are seen in association with HIV infection. The most common variety is a severe form of the recurrent aphthous ulceration, which is seen the general population. Aphthous ulcers (Figure 8), also known as canker sores, are not contagious. Other causes of oral ulcers that have been mentioned include lymphoma, herpes group virus infections, mycobacterial ulcers, and, rarely, fungal ulcers caused by histoplasma and cryptococcus. In addition, NUP and a variant that affects soft tissue, necrotizing stomatitis, must be considered in the differential diagnosis. The appearance of some oral ulcers is consistent with recurrent aphthous ulcers. Others are larger, may not be recurrent, and may fall into the category of necrotizing stomatitis. Recurrent aphthous ulcers may range in size from 1 mm to 5 mm for minor aphthae, to as much as 2 cm for major aphthae. The latter may be very persistent and painful and can interfere with speech and swallowing. A typical aphthous ulcer has a red halo and regular margins and is covered with a grayish pseudomembrane.
Recurrent aphthous ulcers have been treated with topical steroids such as fluocinonide 0.05% ointment mixed with equal parts Orabase® which has 20% benzocaine, and applied six times daily; clobetasol 0.05% ointment mixed with equal parts of Orabase® and applied three times daily; or dexamethasone elixir 0.5 mg/5 ml used as a mouth rinse two to three times per day and expectorated. However, thalidomide has recently been approved for this indication, but still contraindicated for pregnant women.
Salivary Gland Disease and Xerostomia. Complaints of dry mouth in HIV-infected people are often caused by medications that interfere with salivary secretion, such as antihistamines, anti-anxiety medications, antidepressants, and didanosine, an HIV medication. Other patients may experience enlargement of the major salivary glands with or without xerostomia. This is associated with a CD8 lymphocyte infiltration of salivary glands and sometimes other organs; it is also associated with a slightly slower progression of HIV disease. Management of xerostomia should include sucking on sugarless candies or chewing gum and using salivary substitutes. Some patients may benefit from the stimulation with pilocarpine (5 mg, three times a day). Use of topical fluoride rinses should be encouraged to prevent an increase in caries.
Complications
People infected with HIV eventually develop symptoms that usually last a long time and are often severe. Known as AIDS related complex, these symptoms include enlarged lymph glands, fever, tiredness, loss of appetite and weight loss, diarrhea, and night sweats and some of the oral complications already mentioned. As the immune system becomes weaker, the infected person becomes more susceptible to illnesses that normally do not occur in healthy people. They take advantage of damage to the immune system and rarely occur in people with a healthy immune system.
Dental healthcare professionals must stay current on their knowledge of HIV-related infections. The CDC has developed guidelines in conjunction with U.S. Public Health Service and the Infectious Diseases Society of America (IDSA) for the prevention of opportunistic infections among HIV-infected individuals. The report gives guidelines specific to each type of opportunistic infection.
• Pneumocystis jiroveci; formerly known as Pneumocystis Carinii Pneumonia (PCP)
• Cytomegalovirus infection (CMV)
• Toxoplasmosis
• Cryptococcosis
• Tuberculosis
• Candidiasis
• Kaposi's sarcoma
• Mycobacterium avium complex (MAC)
• Cryptospoidium enterocolitis
• HIV dementia
• Malignancies (cancers)
• HIV lipodystrophy
• Chronic wasting (involuntary weight loss and physical deterioration) from HIV infection
TB and HIV
People infected with HIV and TB have a 100 times greater risk of developing active TB and becoming infectious compared to those people who are not infected with HIV.
CDC estimates that 10% to 15 % of all TB cases and nearly 30% of cases among people 25 to 44 years of age are occurring in HIV infected individuals. Therefore the following guidelines for the treatment of HIV-related TB have been developed.
• Directly observe therapy (DOT) for all patients with HIV-related TB.
• Improved prognosis with the use of potent antiviral therapy.
• The use of a 6 month regimen consisting of an initial phase of isoniazid, pyrazinamide, and ethambutol given 2 months followed by isoniazide and rifabutin for 4 months. Prolonged treatment up to 9 months for patients with a delayed clinical or bacterial response to therapy with cavitary disease on chest radiograph.
• Rifabutin-based regimens given at least three times a week for patients with TB and advanced HIV.
• Children and pregnant women with HIV related TB require special considerations.
Screen Testing
Enzyme immunoassay (EIA) is a screening test for HIV. A blood sample is drawn, sent to a lab, and the results are available within several days to several weeks. A negative screening test means a person is not infected with HIV, and does not require further testing. If a person engages in risky behaviors they could be in the window period and a repeat test is suggested in six months. A positive screening test means the person needs further testing. A Western Blot, or immunofluorescence assay (IFA), is performed to confirm the diagnosis of HIV.
A rapid test licensed by the Food and Drug Administration (FDA), known as the Single Use Diagnostic System for HIV-1 (SUDS) can give HIV-1 test results in 5 to 30 minutes. Another rapid test is OraQuick ADVANCE® HIV-1/2 Test detecting antibodies to HIV-1 and HIV-2 in 20 minutes. The OraQuick test was approved by the FDA to use with oral fluids. A reactive HIV test result from either of these tests needs to be confirmed by a Western blot.
The patient having a rapid test can be advised immediately of their screening test results, and counseled on HIV prevention and transmission. A negative rapid test result is always negative, unless the patient has been tested before the antibodies have formed (window period).
HIV Transmission
The blood, semen, vaginal fluid, and breast milk of people infected with HIV has enough of the virus in it to infect other people. According to aids.gov, there is not enough HIV in feces, nasal fluid, saliva, sweat, tears, urine, or vomit to infect another person, however, unless they become mixed with blood and come in direct contact. The CDC has kept saliva on the list of body fluids that require the healthcare professional to exercise standard precautions due to that fact. The CDC and the American Dental Association's Council on Dental Therapeutics suggest assuming that saliva containing a lot of blood could potentially carry HIV and other harmful pathogens.
An HIV infected person who has no signs of an infection or illness can still infect others. There are five known common ways HIV is transmitted:
1. sexual intercourse where fluids can enter through microscopic skin breaks or sores caused by herpes or syphilis;
2. sharing needles and syringes during injected drug use;
3. occupational exposures through eyes, mouth, or open sore;
4. babies born of infected mothers and drinking breast milk of infected mothers;
5. as a result of a blood transfusion or organ transplant from an infected donor.
HIV can enter the body through certain types of tissues that line the anus, vagina, or penis. It also can enter through cuts or tears in the vagina, rectum, penis, or mouth. HIV can be spread through unprotected sexual intercourse from male-to-male, male-to-female, or female-to-female. Unprotected sexual intercourse means sexual intercourse without correct and consistent use of a latex, polyurethane, or polysoprene condom. Lambskin condoms will not protect the users as the virus is small enough to penetrate through it. Even then, condoms do not provide 100% protection from sexually transmitted diseases, but users are always safer. It is possible to contract HIV through oral sex if there are open sores in a person's mouth or bleeding gums.
Insects such as mosquitoes, bugs or animals do not spread HIV. HIV is also not spread through casual contact of any kind such as:
• sharing a telephone,
• toilet seats/doorknobs,
• sharing dishes; or
• holding hands or hugging.
Prevention
Reducing high risk behaviors through educational efforts can prevent HIV infections. To prevent HIV infections, the (CDC) offers the following suggestions:
• do not have sex with an HIV-infected person,
• do not share needles with an HIV-infected person, and
• avoid any risky behaviors that might result in contact with blood, semen, vaginal secretions, or other body fluids.
The best way for a healthcare worker to avoid contracting HIV and developing AIDS is to follow CDC's recommendations to treat "every patient" as though they are HIV+. The Occupational Health and Safety Administration (OSHA) and CDC recommend the use of standard precautions whenever there is a risk of a person being exposed to contaminated blood or body fluids. It is recommended that all individuals be treated as if they could be infected. Hand washing is the single most important factor in preventing HIV and other diseases. Keeping hands away from one's face and not eating or drinking in any environment that may be contaminated is recommended.
Barrier precautions should always be used to prevent exposure to blood and other body fluids. Vinyl or latex gloves must be worn before touching any blood, body fluids, non-intact skin, mucous membranes, or excretions. Safety glasses are worn over the eyes and a mask covering the mouth and nose are in place to protect from possible spatter into exposed mucous membranes. Wearing a clean, waterproof, non-sterile gown will protect the healthcare worker from exposure to contaminated body fluids. Both OSHA and CDC recommend the use of blood and body fluid precautions for all invasive procedures. An invasive procedure is a procedure requiring surgical entry into tissues, organs, cavities, or repair of traumatic injury. These precautions prevent the transmission of pathogens from all body substances. When performing CPR, masks, ventilation bags, and other intubation equipment should be used to prevent exposure to bloody saliva.
The most direct way of spreading HIV is through a puncture wound from a contaminated needle or other sharp object that causes a break in the skin. Engineering controls and work practice controls must be in place to prevent needle sticks. Controls such as needle guards and protective sheaths and one-handed scoop techniques are options for minimizing sharps injuries. Needles should NEVER be bent, broken, or removed from contaminated syringes. Sharps should be disposed into a puncture-proof container and then transported to a reprocessing area. One out of every four needle stick injuries involves IV therapy equipment.
Specimens should be placed in leak-proof bags or containers with an identifiable biohazard warning label. Used equipment and instruments need to be systematically cleansed and sterilized. HIV droplets can "easily be destroyed" on surfaces by exposure to common cleansing agents and by all routine methods of sterilization.
It is important to use OSHA guidelines and to have an Exposure Control Plan that is available to all employees with potential occupational exposure to infectious diseases and other health hazards. Procedures related to the proper cleansing of and disinfection of all floors, walls, bathrooms, bed, bedside furniture and other items used by the nurses, doctors, clients and visitors are adequate enough to prevent the spread of HIV. Annual training programs should include the following components:
• Epidemiology and symptoms of HIV
• Modes of transmission
• Explanation of the exposure control plan
• Training in universal precautions
• Engineering controls
• Safe work practices and personal protective equipment
• Explanation of procedures and follow-up
• Explanation on bio hazardous waste signage and labeling
Significant Exposure
As of December 2010, there were 57 documented cases, and 143 possible transmissions of occupational HIV transmission to health care workers in the United States. There are no confirmed cases reported since 1999. Occupational transmission of HIV is voluntarily reported in the Centers for Disease Control and Prevention. Healthcare workers and non-medical personnel who are providing emergency medical assistance or are on the job experiencing a significant exposure are entitled to know the HIV status of the source client. This information can be obtained as follows:
| 1. | From the source client's medical record if his HIV status is documented. | |
| 2. | If the test results are not available, the blood of the source client can still be tested "without consent" in these situations: | |
| • | When the blood sample from the source was drawn voluntarily for another purpose prior to the exposure. | |
| • | When the blood sample was drawn during the course of treatment for medical emergency. | |
| 3. | Procedures to follow if after asking the source for consent if he/she does not want to give consent or is unable to give consent due to his/her physical status. | |
| • | The physician has to document that a significant exposure has occurred and that those exposed need the test results to determine if treatment is needed. Documentation may not be placed in the medical record of the source client. | |
| • | The exposed person's blood must be tested or a negative test result obtained within the past six months. | |
| 4. | There is a special provision giving the medical examiner or attending physician the authority to test a deceased source's blood if there has been a significant exposure. | |
Prompt initiation of antiretroviral therapy soon after occupational exposure to HIV was found to substantially reduce the risk of HIV seroconversion. Therefore, the U.S. Public Health Service recommends Post-exposure prophylaxis (PEP) with antiretroviral agents for anyone exposed to HIV during a single event. This includes a sharps injury, infectious fluids contamination in the eye, mouth, or open skin. These medications are only available with a prescription. PEP should begin as soon as possible, and must be within 72 hours. Research has shown little or no effect if started more than 72 hours after HIV exposure.
PEP treatment is with two or three antiretroviral medications for four weeks if tolerated. PEP therapy is not 100% effective and does not guarantee that exposure to HIV will not become a case of HIV infection.
The U.S. Public Health Service does not recommend for or against antiretroviral agents for non-occupational situations because of the lack of efficacy data.
Treatments
Presently there is no cure for HIV. Vaccines are under development but are not yet available. Human testing has begun at the University of Massachusetts.
Medications
As of 2011, there were 24 approved antiretrovirals (ARV) and 6 ARV classes. These provide unprecedented treatment opportunities for both treatment-negative and treatment-experienced HIV+ patients. Treatment paradigms remain unsettled and constantly evolving due, in large part, to new clinical trials and other data that are presented or published. The challenge for the patient's physician and HIV+ treatment provider(s) is to be aware of these trials and other presented or published data. Being knowledgeable of these trials allows an appropriate ARV regimen for each HIV+ patient regardless of ARV experience. Medications need to be potent, tolerable, safe, durable, and, if possible, future treatment options must be maintained. These will be prescribed by the patient's physician, but could be changed often. Therefore, the dental/medical history must be checked and current at all times.
Current treatment consists of medications to slow down the process of HIV duplication and weakening of the body's immune system. Highly Active Anti-Retroviral Therapy (HAART) is the combination of three or four antiretroviral agents.
The following are a list of medications that may be used in HAART:
Nucleoside/Nucleotide Reverse Transcriptase Inhibitors (NRTIs)
• zidovudine (AZT, ZDV) (Retrovir®)
• didanosine (ddI) (Videx®)
• lamivudine (3TC) (Epivir®)
• stavudine (d4T) (Zerit®)
• tenofovir (Viread™)
• zalcitabine (ddC) (HIVID®)
• abacavir (Ziagen™)
• zidovudine +lamivudine (Combivir™)
• zidovudine+lamivudine+abacavir (Trizivir®)
Protease Inhibitors (PIs)
• saquinavir (Invirase™ & Fortovase™)
• ritonavir (Norvir™)
• indinavir (Crixivan®)
• nelfinavir (Viracept®)
• amprenavir (Agenerase®)
• ritonavir/lopinavir (Kaletra™)
Non-Nucleoside Reverse Transcriptase Inhibitors (NNRTIs)
• nevirapine (Viramune®)
• delavirdine (Rescriptor®)
• efavirenz (Sustiva™)
The success of this therapy is dependent not only on the HAART treatment plan, but also on the patient's ability to strictly adhere to the new medication regimen and tolerate the side effects of these powerful drugs. Side effects that may seem minor, such as fever, nausea, and fatigue, can mean there are serious problems. It is important for the healthcare team to be aware of side effects. More serious side effects of HAART treatment plans are:
• liver problems;
• diabetes;
• fat maldistribution;
• high cholesterol;
• increased bleeding in patients with hemophilia;
• decreased bone density; and
• skin rash.
In the hospital or dental setting, the CDC does not recommend special isolation for HIV/AIDS patients unless a highly contagious and transmissible disease is present. It is not acceptable to identify or flag a patient with HIV/AIDS in any way that is different from any other patient. Patients with HIV/AIDS may have other conditions that require isolation, such as tuberculosis, infectious diarrhea, or other communicable diseases. Isolation procedures in these cases should be applied as they would be done for any other patient.
Nutritional Care
One area that is often overlooked is the nutritional state of the person who is HIV+ or diagnosed with AIDS. Nutritional care is a vital, integral, and cost effective way to improve the overall health status of a person who is diagnosed HIV+/AIDS. HIV/AIDS patients can be empowered to manage the nutritional aspect of self-care. Malnutrition is often associated with HIV/AIDS disease. Malnutrition develops because the body has a greater need for calories, protein, vitamins and minerals. These increasing nutritional demands can be due to pregnancy or fever. Many people who are suffering from malnutrition have a decreased desire or tolerance for healthy foods due to the following:
• pain (sore mouth) due to opportunistic infections, candidiasis, and poor dentition;
• decreased appetite due to illness, drug-related anorexia, nausea and vomiting, and taste changes;
• neurological complications due to dysphasia, dementia, and lack of coordination;
• financial barriers due to homelessness, jobless, and lack of insurance;
• problems with food access due to fatigue, disability, lack of social support, and lack of transportation;
• malabsorption due to HIV-related changes in the GI tract, HIV drugs with side effects of diarrhea, nausea, and vomiting;
• substance abuse.
The standard of care for the HIV/AIDS person is that nutrition should be guided by a registered dietitian. The dietitian does a baseline nutritional assessment, dietary counseling, on-going assessments, counseling and aggressive interventions as indicated. The dietitian also provides diet-drug counseling, like timing of medications versus food intake and symptom management.
The following are brief dietary guidelines that the dietitian considers in providing care to the HIV/AIDS client. To decrease cholesterol a standard heart healthy diet should be followed. Listed is what is suggested to be generally effective:
• <30% of calories from fat;
• limit saturated fats;
• high fiber diet;
• aim for monosaturates;
• possible use of lipid lowering agents;
• caution with exercise due to possible infarcts occurring.
To achieve or maintain glycemic control the following has been recommended:
• low fat diet;
• no concentrated sweets; and
• consistency in amount and timing of carbohydrates.
Doctors may also prescribe appetite stimulating and anabolic agents. Exercise should be encouraged to increase the patient's strength/muscle mass and referral to a physical therapist may be necessary.
Social workers can assist to ensure that the client has access to a safe and nutritious supply of food and that the members of the healthcare team continue to work together to improve the quality of life of the person who has HIV or AIDS.
Ethical Dilemmas
AIDS is a worldwide stigmatized disease and, because of this, people with AIDS may not be willing to seek treatment and may not follow the treatment plan. The patient requires emotional, physical, and psychological support. How one became infected is not as important as dealing with this life threatening, debilitating disease. Censure and condemnation are not acceptable when providing care for the individual with this disease. Caregivers must have the inner strength and fortitude to provide hope, compassion, and respect to the AIDS patient as his or her disease progresses. In the terminal stages, increasing physical and emotional support are required.
In the hospital setting, the CDC recommends special isolation for an AIDS patient only if conditions such as tuberculosis, infectious diarrhea or other communicable diseases are present. Clinical assessment should focus on identifying and treating the infection, maintaining functioning organs, providing symptomatic relief of discomfort, preventing and treating complications, and most importantly, providing physical and compassionate emotional support to the patient, his or her family, and/or significant other.
Living With HIV
The CDC recommends routine HIV screening for adults and adolescents, including pregnant women, in health care settings in the United States and recommends reducing barriers to HIV testing.
Elderly
The recommendations specify routine testing for people up to age 64. People aged 64 and over should be counseled to receive HIV testing if they have risk factors for HIV infection.
Routine testing is intended not only to identify persons who are unaware that they are HIV+ but also to remove the stigma of being tested. Making testing routine for older people can help open a discussion between a physician and an older person concerning at-risk behaviors.
Prevention strategies should be developed for older people who are potentially at risk for HIV infection. This can include education to increase awareness and knowledge, skills training to help them negotiate risk-reduction behaviors, and messages that are age-appropriate and culturally sensitive. Intervention strategies to help older women negotiate safer sexual behaviors are especially important.
A recent review of HIV/AIDS behavioral interventions for people 50 years and older recommended simultaneous, multilevel approaches including building on the current understanding of behavioral changes and HIV prevention successes with younger populations while considering important intervention principles gathered from work with older populations in other health areas.
Women
One in four people living with HIV infection in the U.S. are women. Among women ever diagnosed with AIDS, an estimated 4,014 died during 2010, and by the end of 2010, an estimated 111,940 had died since the beginning of the epidemic. Most of the AIDS cases in adolescents are young women who are of African and Latin American decent. Due to the prolonged incubation period from HIV infection to the time of an AIDS diagnosis, it is probable that infection occurred during adolescence. Most new HIV infections in women are from heterosexual intercourse (84%).
Recent studies have shown that women with AIDS survive a shorter time than men when they are diagnosed later in the disease process. This may be due to limited access to or use of healthcare resources, homelessness, domestic violence, and lack of community support. The most common cause of death in HIV+ women was due to bacterial pneumonia, pneumocystis jiroveci, and toxoplasmosis. Women also demonstrated a higher incidence of candida infections, chronic or recurrent mucocutaneous herpes and simplex infections.
HIV transmission from mother to child during pregnancy, labor/delivery, or breastfeeding is known as perinatal transmission. This is the most common route of HIV infection in children. When HIV is diagnosed before or during pregnancy, perinatal transmission can be reduced to less than 1% if appropriate medical treatment is given, the virus becomes undetectable, and breastfeeding is avoidable. Studies suggest that HIV+ pregnant women start medications early, after discussing with their treating physician, to decrease to amount of virus in the bloodstream at the time of delivery. However, those in their first trimester may want to delay initiation of therapy until after 10-12 weeks of gestation since this time is the most susceptible to the potential teratogenic effects of drugs.
One way of decreasing HIV transmission to the newborn begins with having the baby and mother tested prior to delivery. Naturally, the mother has to consent and the procedure must be explained to the mother at her level of understanding. If there is a possibility that the baby will contract HIV, experts are now recommending several medications to reduce the newborn's chances of acquiring HIV. One medication is zidovudine, better known as AZT, and it is given intravenously through the mother. The other is an oral drug called nevirapine in the form of Viramune®. After the baby is born the doctor may place the newborn on AZT syrup. These medicines have been studied for use in pregnant women and newborns, and there have been no serious long term side effects.
Short term side effects that may occur with AZT are vomiting, headache, fatigue, anemia (low red blood cell numbers), decreased number of white blood cells (these are the cells that fight infection), loss of appetite, heartburn, trouble sleeping. Side effects of nevirapine can be skin reactions or problems with the liver.
The tragedy of HIV is that few women are not aware of their illness until their child becomes ill. Now, the CDC has advocated universal counseling and testing for every pregnant woman regardless of geography, identified risk behavior, or self-identified risk. A pregnant woman may decline these services and the healthcare provider must document this has occurred.
Legal Information for the Healthcare Provider
Many states, as well as the federal government, have enacted statutes and regulations related to the care of patients diagnosed with HIV and AIDS. Addressed are topics dealing with the documentation of HIV/AIDS and related diagnosis, issues of informed consent, and the maintenance of patient confidentiality.
Confidentiality
Strict patient confidentiality is required by the dental team for all patients, including those diagnosed with HIV and AIDS. No one has the right to disclose a patient's positive HIV status or testing information. Results may only be given to the person tested or the legally authorized representative.
Legal release includes:
• a specific release when the test subject, in writing, specifically authorizes the release of his/her HIV status to a third party payer or specifically named person.
• a prior written authorization to honor a general release that is signed at the time the test is done.
The Omnibus AIDS Act limits access to HIV test results to those taking care of the individual and those who have to have a need to know. The act allows for a specific disclosure permitted by statute or administrative rule in the following situations:
• to healthcare providers involved in the treatment and care of the test subject and in the course of having to consult with other healthcare professionals/facilities to determine treatment or diagnosis;
• to a healthcare provider involved in the delivery of a child may note the mother's HIV status in the newborn's medical record;
• to the Department of Health to comply with reporting rules;
• to authorized authorities when reporting child abuse;
• to those adults who are responsible for a child who is placed in foster care or is for adoption;
• to those facilities and providers engaged in the transfer of body parts and tissues;
• to employees of community based care programs or residential facilities for developmentally disabled individuals when they are directly involved in the care, control, or custody of the resident.
The Omnibus AIDS Act prohibits the release of a medical record with an HIV test result in response to a subpoena. There must be a court order, signed by a judge.
The Omnibus AIDS Act provides that if the healthcare practitioner, including doctors, nurses, social workers, psychologists, mental health counselors, and others find it necessary to notify a partner of the client's HIV status, the practitioner must adhere to a protocol established by the Department of Health. Once this protocol is followed the practitioner is immune from civil and criminal liability.
The Protocol is as follows:
• only the client can identify the third party;
• the healthcare practitioner must encourage the client to notify his/her partner or use the Department of Health's partner notification program;
• if the client refuses, the practitioner advises the client that they are going to notify the partner;
• the preceding must be documented without the name of the third party.
Infection Control
While a dental professional can cross contaminate to others, the major source of the microorganisms in dental offices is the patients' mouths. It is not possible to accurately detect which patients may indeed be harboring germs, especially with a virus like HIV that has a long window and incubation period. To successfully prevent the spread of pathogens, infection control procedures must be applied during the care of all patients using the concept of standard procedures - considering all patients to be infectious. The importance of standard precautions is based on the understanding that asymptomatic carriers of a disease can be highly infectious.
Protecting Patients
The CDC, OSHA, as well as all dental professional organizations, have recognized the importance of protection against bloodborne pathogens.
Cross-contamination from a member of the dental team to a patient is a relatively rare event in dentistry. The overwhelming majority of patient visits do not result in infection. Chances can be reduced even further through the proper application of infection control methods.
Cross-contamination from one patient to another patient may occur by indirect routes through contaminated instruments, surfaces, equipment or even the hands of dental personnel. The goals of instrument are to prevent transfer of infectious agents to patients from contaminated dental hand instruments and handpieces, protect the staff that must handle the items, and consistently fulfill protocols to provide sterile instruments chairside.
Protecting Dental Professionals
Cross-contamination from patient to the dental team mainly involves microorganisms present in the patient's mouth in oral fluids like saliva, blood, oral open lesions. Exposure can occur by direct contact, through dental aerosols and body fluid spatter and by contact with previously contaminated instruments, surfaces and supplies. In the absence of adequate protective measures, the dental team is exposed to the risk of infection by oral bacteria and bloodborne pathogens present in the patient's mouth. The risks are real, as dental personnel are known to acquire occupational exposures at rates much higher than the general population.
Practitioner safety can be increased by the proper sterilization of reusable instruments. Correct disinfection and/or covering of environmental surfaces likely to be orally soiled will decrease the risks for both practitioners and patients. The proper use of personal protective equipment (PPE) can minimize exposure to patient germs (Figure 9).
In the past, protection of employees from bloodborne pathogens primarily involved selection of PPE, such as gloves, masks and protective eyewear. Although PPE is an essential component of an infection control and occupational safety program, it is not considered to be a first-line defense against occupational exposures. For example, wearing examination gloves does not fully protect employees against needlestick accidents. OSHA has indicated that engineering, work practice, and administrative controls are to be used to eliminate or reduce employee exposures. If occupational exposures remain after the application of controls, PPE should also be used.
Engineering controls are considered the most effective manner to prevent occupational exposures. Engineering controls isolate or remove a hazard from the workplace. In the case of sharps devices, safety features or engineering controls prevents sharps contaminated with patient blood from contacting employees. Examples would include sharps disposal containers (Figure 10), self-sheathing needles, safer medical devices, such as sharps with engineered sharps injury protections and needleless systems. Employers in dental practices must select and implement appropriate engineering controls to reduce or eliminate employee exposure.
Work practice controls reduce the likelihood of exposure by altering the manner in which a task is performed. Prohibiting two-handed recapping of contaminated needles is a work practice control. Work practices involve training employees on how to perform necessary tasks in ways that reduce their exposure to workplace hazards. OSHA requires employers to identify and administer safer work practices.
Sometimes considered part of work practice controls, administrative controls involve changing how or when employees do their jobs. Examples include scheduling work and rotating employees to reduce exposures, posting written safety policies, and requiring the whole staff to follow the safety rules. Although the practice of dentistry does not easily lend itself to administrative controls, changing the timing of some work tasks could reduce the numbers of employees potentially exposed to a hazard.
OSHA's Bloodborne Pathogens standard, including the 2001 revisions, applies to all employers who have any employee with a possibility of occupational exposure. Every employer must keep an updated Office Exposure Control Plan and keep a Sharp's Injury Log. They must uphold all standard precautions, establish work practice controls, and promote proper hand hygiene and PPE use.
Protecting the Community
Two other routes of microbe spread involving dental offices to community include improper handling of regulated medical waste (e.g., improper containment of contaminated medical waste, including sharps during transport) and sending orally contaminated dental impressions or appliances to a dental laboratory. Medical wastes in many areas can be treated (sterilized) in-house, decreasing the chances of cross-contamination. Or, a commercial waste hauling service could be hired. Impressions and appliances should be disinfected properly before being sent out and upon being received back into the office.
Summary
The prevalence of HIV/AIDS is still affecting millions of people. Rapid changes are taking place in HIV/AIDS treatment. The extension of life expectancy among people with HIV/AIDS provides healthcare workers, educators, scientists, and the dental healthcare team with the opportunity to enhance the quality of life among those who are afflicted with this disease.
It is the responsibility of all healthcare providers to be educated on the current treatment of HIV/AIDS patients. Research is being done nationally and worldwide toward the advancement of drug therapies. The dental team must be aware of these therapies and also discuss possible nutritional care. As oral examinations are performed, the dental team must look for oral manifestations that can aid in diagnosis and overall patient treatment.
Dental professionals must not be afraid to ask questions of their patients. This concept ensures that we are providing the best possible care for patients. It is imperative to maintain all HIPAA principles concerning patient confidentiality.
Easy access to prevention and treatment sites without the fear of condemnation will enhance our ability as a society, to keep us all safe from this deadly disease.
Glossary
+ - stands for positive
- - stands for negative
acquired immunity - resistance resulting from previous exposure to an infectious agent or antigen, may be passive or active
active immunity - protection from a disease as a result of previous exposure to the disease-causing agent or antigens; defense may also result from vaccination
antibodies - protein-rich molecules dissolved in blood and other body fluids that can destroy antigens
antigens - materials foreign to a human; generally can elicit an immune response by itself
cytomegalovirus - (CMV) an opportunistic herpes-family virus; no cure or vaccination exists; can affect eyes, sight, and salivary glands
DNA - deoxyribonucleic acid; molecular chain found in genes within nuclei of cells; carries genetic information; principle constituent of chromosomes
engineering controls - controls that isolate or remove a hazard from the workplace
HAART - combination of several (typically three or four) antiretroviral drugs is known as Highly Active Anti-Retroviral Therapy (HAART); combined use of at least two reverse transcritpase inhibitor drugs and a protease inhibiting drug
hypochlorhydria - state where the production of gastric acid in the stomach is absent or low
Kaposi's sarcoma - (KS) a common opportunistic cancer associated with HIV causing purple, red, or brown lesions on the skin, nose, oral tissues, and organs
lymphocyte - white blood cell; present in blood, lymph and lymphoid tissue
macrophage - large immune cell that collects and devours invading pathogens and other invaders; large amounts of HIV can be harbored inside without adverse effect; serve as reservoirs of HIV
NUP - necrotizing ulcerative periodontitis; a marker of severe immunosuppression that affects gingival tissues (gums) and extends to the underlying bone or periodontium
opportunistic - illnesses that normally do not occur in healthy people but become problematic to those with a weakened immune system
palliative - relieving pain
passive immunity - transfer of short-acting immunity from one person to another
pastille - sweet medicinal pill made of a thick liquid; absorbs into the mucous membrane
phagocyte - a type of cell capable of engulfing and absorbing bacteria and other small cells
Pneumocystis jiroveci - pronounced "yee-row-vet-zee," formerly known as Pneumocystis Carinii Pneumonia (PCP); a common opportunistic virus affecting the lungs
prevalence - a measure of the proportion of people in a population affected with a particular disease at a given point in time
prodromal - the period of time between initial infection and full development of symptoms
retrovirus - use reverse transcriptase to convert RNA to DNA, which then become part of the host cells' genetic material
RNA - ribonucleic acid; nucleic acid usually found in the cytoplasm of cells; structurally similar to DNA
sequestration - referring to withdrawal or separation
teratogenic - related to, or causing developmental malformations
toxoplasmosis - a parasitic disease affected people with compromised immune systems; associated with under cooked foods and unclean eating utensils
troche - a lozenge that dissolves slowly as it is held between the tongue and mucous membrane
work control practices - controls that reduce the likelihood of exposure by altering the manner
References
AIDS Info Net fact sheets. Retrieved March 2013 from www.aids.infonet.org
AIDS/Meds.com. Trizivir. Retrieved March 2013 from http://www.aidsmed.com/drugs
AIDS/Meds.com. Combivir. Retrieved March 2013 from http://www.aidsmed.com/drugs. Combivir.htm.
Centers for Disease Control and Prevention. HIV/AIDS statistics and surveillance: basic statistics 2011. Retrieved March 2013 from: http://www.cdc.gov/hiv/topics/surveillance/basic.htm
CDC. Monitoring selected national HIV prevention and care objectives by using HIV surveillance data-United States and 6 U.S. dependent areas-2010. HIV Surveillance Supplemental Report 2012;17(No. 3, part A). Published June 2012.
CDC. Estimated HIV incidence among adults and adolescents in the United States, 2007-2010. HIV Supplemental Report 2012). Available at http://www.cdc.gov/hiv/topics/surveillance/resources/reports/index.htm#supplemental.
CDC Fact sheet: Estimates of New HIV Infections in the United States. Retrieved March 2013 from http://www.cdc.gov/hiv/topics/surveillance/resources/fact sheets/incidence_overview.htm.
CDC. HIV Prevalence Estimates. Retrieved March 2013 from: http://www.cdc.gov/hiv/topics/surveillance/basic.htm.
CDC. HIV/AIDS Among African Americans. Retrieved March 2013 from http://www.cdc.gov/hiv/pubs/facts/afam.htm.
CDC. HIV Surveillance 2010 Update Retrieved March2013 from http://www.cdc.gov/hiv/pubs/facts/afam.htm.
CDC. (n.d.b). HIV and its treatment: What you should know (2nd ed.). Center for Disease Control, National Center for HIV, STD and TB Prevention, Divisions of HIV?AIDS Prevention. Retrieved March 2013 from http://aidsinfo.nih.gov/guidelines/adult/brochure/.
CDC. (n.d.a). OraQuick rapid HIV test for oral fluid-frequently asked questions. HIV/AIDS Among African Americans. Retrieved March 2013 from http://www.cdc.gov/hiv/pubs/facts/afam.htm.
CDC. Surveillance of healthcare personnel with HIV/AIDS. HIV/AIDS Among African Americans. Retrieved March 2013 from http://www.cdc.gov/hiv/pubs/facts/afam.htm.
CDC. Testing Makes Us Stronger. Retrieved February 2014 from http://hivtest.cdc.gov/stronger/hiv/index.html
CSC Health Disparities and Inequalities Report - United States 2011.
Goldrick, B., Baigia, J., Larsen, J., & Lemert, J. (2000). Nursing research and HIV infection: State-of -the-science. Journal of Nursing Scholarship. 32(3), 233-238. Retrieved March 2013 from Proquest.
Greenspan, Deborah, D.D.S. and John S. Greenspan, D.D.S.. Oral Manifestations of HIV infection. AIDS Clinical Care. Vol. 9 No. 4 of, April, 1997. Accessed March 2013. http://www.hivdent.org/_oralmanifestations_/Oral Manifestations of HIV Infection.
Hall HI, Ruiguang S, Rhodes P, et al. Estimation of HIV incidence in the United States. JAMA. 2008; 300:520-529.
Marks G, Crepaz N, Janssen R. Estimating sexual transmission of HIV from persons aware and unaware that they are infected with the virus in the USAA. AIDS. 2006; 20:1447-1450. Retrieved March 2013 from http://aidsonline.com/pt/re/aids/fulltext
Pinkerton, S., Martin, J., Roland, M., Katz, M. et al. (2004). Cost-effectiveness of post exposure prophylaxis after sexual or injection-drug exposure to human immunodeficiency virus. Archives of Internal Medicine. 164(1). P 46-56. Retrieved CDC. (2003b). HIV/AIDS Among African Americans. Retrieved March 2013 from Proquest. http://www.cdc.gov/hiv/pubs/facts/afam.htm.
Reznick, David A., D.D.S., O'Daniels, Christine, RN-BC. Oral Manifestations of HIV/AIDS in the HAART Era. www.hivdent.org/_oralmanifestations_omhah0502.htm.
The Immune System. The Ohio State University: Wexner Medical Center. Retrieved February 2014 from http://medicalcenter.osu.edu/patientcare/healthcare_services/infectious_diseases/immunesystem/Pages/index.aspx
Thomas, Donna. HIV/AIDS for the Healthcare Professions.
Trynka, S., & Erlen, J. (2004). HIV disease susceptibility in women and the barriers to adherence. Medsurg Nursing, 13(2), p13 (2), p 97-105. Retrieved July 24, 2012 from Proquest 13(2), p 13(2), p 97-105. UNAIDS Epidemic Update 2010 Retrieved March 2013 from http://www.unaids.org
UNAIDS Epidemic Update 2008 Retrieved March 2013 from http://www.unaids.org
ABOUT THE AUTHORS
Janet Tuthill, RDH, MA
Lead Author, Janet Tuthill, RDH, MA is Director of the Dental Assistant Program at Stony Brook University, School of Dental Medicine in Stony Brook, New York. Her recent publications include research on the role of allied dental health care providers in HIV and diabetes screening as well as issues related to access to care.
Wilhemina Leeuw, MS, CDA
Contributing Author, Wilhemina Leeuw, MS, CDA is a Clinical Assistant Professor of Dental Education at Indiana University Purdue University, Fort Wayne. A DANB Certified Dental Assistant since 1985, she worked in private practice over twelve years before beginning her teaching career in the Dental Assisting Program at IPFW. She is very active in her local and Indiana state dental assisting organizations. Prof. Leeuw's educational background includes dental assisting - both clinical and office management, and she received her Master's degree in Organizational Leadership and Supervision. She is also the Continuing Education Coordinator for the American Dental Assistants Association.