You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
While per capita consumption of cigarettes continues to decline among adults and is leveling off in teenagers, spit tobacco consumption is on the rise. The most recent epidemiological data shows that over 750,000 adolescents use spit tobacco on a regular basis. According to the 2011 Youth Risk Behavior Surveillance System from the Centers for Disease Control (CDC) National Center for Chronic Disease Prevention and Health Promotion, 7.7 % of high school students used spit tobacco products in the last 30 days. This figure doubles, for white, male high school students, to 15.6%. Even as the popularity of this known carcinogen reaches record levels among young people, spit tobacco use continues to get relatively little attention as a public health issue. The image marketed by the spit tobacco industry of spit tobacco as a safer substitute for cigarettes continues to permeate many sections of society.
The need for education among the general public is immediate. Oral Health America's National Spit Tobacco Education Program (NSTEP) worked closely with the Robert Wood Johnson Foundation, the CDC, and Major League Baseball (MLB) from 1994 to 2005. (Neither NSTEP or OHA are currently affiliated with CDC or MLB.) During this time a nationwide network of spit tobacco education and cessation resources were developed. The goal of NSTEP and its partners continues to be to prevent the youth from becoming lifelong users of tobacco through achieving reductions in the experimentation and regular use of spit tobacco. The message that spit tobacco is not a safe alternative to cigarettes must become woven into the cultural fabric of mainstream America. Exposing youth, their role models, health care professionals, and opinion makers in a wide variety of cultural, social, and entertainment contexts to the anti-spit tobacco message can accomplish this objective. The dental team is in an ideal position to use the "teachable moments" that occur during a dental visit to counsel their patients on the dangers of tobacco use while supporting them in their cessation efforts.
Basics of Spit Tobacco
Types of Spit Tobacco
Spit tobacco, also known as smokeless tobacco, comes in two forms: chewing tobacco and snuff. The products differ with regard to type and part of the tobacco plant used, method of curing and processing, moisture content and additives. Snuff is often referred to as "dip" and, at present, is the most popular type of spit tobacco sold in the U.S. It is produced in two varieties, moist and dry, and is packaged in loose and packed forms. While snuff users in the U.S. prefer the moist type, dry snuff use can still be found in population groups such as the elderly and tobacco users outside of the United States.
Snuff. Dry snuff is produced from fire-cured tobacco. This tobacco is fermented after the curing process, allowed to dry and finely ground into a powder. With moisture content of less than 10%, dry snuff can be inhaled through the nose or placed in the mouth between the cheek and gum.
Moist snuff is produced from tobacco that has been either air or fire cured, processed and finely ground or cut. The moisture content can be up to 50%, allowing the user to pinch a small amount of the tobacco or "dip" and place it between the lip or cheek and the gingiva. In addition to the processed tobacco leaves, moist snuff also contains sugar; flavorings, such as cherry, wintergreen and mint; salt; and abrasives such as sand and grit. Moist snuff is sold loose in cans or packaged in premeasured tea bag like packets. Many spit tobacco users dip most of their waking hours and it is not unusual for some to keep a pinch or packet in place 24 hours a day, with young consumers averaging as many as 5 or more dips per day.
Each pinch or packet (depending on the brand) contains the same amount of nicotine as 2 to 5 cigarettes. It is the constant high level of nicotine in the blood that results in the intense addiction found in spit tobacco users.
Chewing Tobacco. Chewing tobacco is sold in three forms: loose leaf, plugs and twists. Loose-leaf chewing tobacco, which is packaged in pouches, is produced from stripped and processed tobacco leaves that are stemmed and then cut or shredded into strips. Sweeteners such as molasses or corn syrup, flavoring, and abrasives are added to achieve the desired texture and flavor. A common flavor in shredded tobacco is licorice. However, some brands of chewing tobacco do not contain any added flavors, resulting in a product that tastes like cured tobacco. The long-term user usually prefers unflavored snuff and chew, while younger and less frequent users will choose one of the flavored products.
Chewing tobacco is also pressed into bricks and sold as plugs. Plugs are firm or moist with a sweet licorice flavor. A third form of chewing tobacco is produced from a dark tobacco leaf, cured, processed and twisted into strands or ropes and dried. Twists are usually manufactured without flavor or sweeteners.
Chewing tobacco is used by taking a portion of the product (called a "quid" or "chaw"), putting it into the mouth, chewing long enough to soften the quid, then placing it between the cheek or lower lip and the gingiva. It is periodically chewed or sucked to extract the nicotine-laden juice. Users of chewing tobacco produce a large volume of tobacco juice or saliva, which must be periodically spit out or swallowed.
History of Chewing Tobacco
It was not until the 15th century and the arrival of Europeans such as Christopher Columbus and Amerigo Vespucci that it was carried to the rest of the world. It was in Europe, especially among royalty and the privileged class, that dry snuff use became popular. It was inhaled by men and women alike who considered its use socially acceptable. By 1570, Europeans were growing a few varieties of tobacco and producing snuff that was eventually exported back to the American colonies.
Tobacco was once so valuable that it could be used as currency. Early on in Europe, tobacco was believed to cure many different ailments. There were several books published on the subject. Tobacco was believed to cure anything from joint pain, epilepsy, and even the plague. Chewing tobacco use was first documented in the 1700's. It was during this time that pipe smoking was also gaining popularity.
By 1789, snuff mills were in operation in the U.S. The first advertisement for snuff and chewing tobacco was for a product called Red Man™, which is still produced today. Its packaging differs little from the pouch of 200 years ago. In the early 1800s, spit tobacco was referred to as "The American Habit." It was common to see communal spittoons in public buildings and to see users spitting on the street and floors. Even the U.S. Congress had communal snuffboxes and cuspidors.
In the early 1900's, spit tobacco use began to sharply decline and became socially unacceptable. This decline was precipitated by three events. One was the belief that tuberculosis could be spread by tobacco juice. The second was the subsequent law against public spitting. The third event was the invention of an efficient cigarette-rolling machine. This allowed for the mass production of inexpensive cigarettes.
Spit tobacco remained a socially unacceptable practice until after the release of the 1964 Surgeon General's report that outlined the health dangers of cigarette smoking. The spit tobacco companies saw this as an opportunity to reintroduce their product as a safe alternative to cigarettes. Thus began intensive mass media advertising using sports figures to show that their product was macho and a component of a successful athletic career. As a result of this very effective campaign, spit tobacco use regained its popularity and has been rising, especially among young people, ever since.
Demographics of Spit Tobacco Use in the United States
Population Statistics
According to the National Survey on Drug Use and Health, in 2011 there was more than 8.2 million users of spit tobacco products. There was no significant decline in the use of any individual tobacco product, including spit tobacco, among high school students from 2002 to 2004. Further, more than 2,200 young people aged 11 to 19 try spit tobacco and 830 become regular users every day. That results in 824,000 young people trying spit tobacco for the first time and 304,000 becoming regular users every year, according to the CDC. If the trend toward increased spit tobacco use among young people continues, the numbers will reach epidemic proportions.
The typical spit tobacco user is a young white male between the ages of 16 and 30 living in the southern part of the U.S. in either a rural or suburban area where spit tobacco is often part of the culture. According to a report by the Surgeon General in 2012, the overall prevalence of spit tobacco among high school age students was 6.7%. The data can be broken down further to isolate the groups with the highest usage. The prevalence of current use was higher among white students (9.5%) than African American (.6%) and Hispanic (2.2%) and among male students (11.6%) as compared to female students (1.8%).
By race, the use of spit tobacco is higher for American Indian and Alaska Native (AI/AN) children than for all other ethnic groups of children. As many as 43% of AI/AN boys and 34% of AI/AN girls use spit tobacco. The National Cancer Institute reports that even preschool aged AI/AN children use spit tobacco. The high usage rates can be linked to a strong cultural and religious history of tobacco use among the AI/AN cultures.
Spit tobacco use by region has shifted. According to recent research, the Midwest has the most users at 4.3% followed by the South at 3.7%, the West with 2.4% and finally the Northeast with 1.9%. Surveys done by the Tobacco Control Research Branch of the NCI found spit tobacco use to be highest in Arkansas, Kentucky, Mississippi, West Virginia, Tennessee, and South Dakota.
In 1970, young men ages 18 to 24 used spit tobacco the least of any age group. Today, usage by this subgroup is the highest of any age subgroup. Spit tobacco has gone from a product used primarily by older men to one which young men comprise the largest portion of the market. For example, in 1970, 12.7% of males 65 or older versus 2.2% of males aged 18-24 years used spit tobacco regularly. By 1991, the use by the younger group rose to 8.4% while the older group decreased its use to 5.6%. A similar pattern is evident for moist snuff use. Spit tobacco use is also being seen in wider and more diverse segments of the population, including young women.
Continued Use
There are many factors contributing to the rise in spit tobacco use among young people. In 1970, the spit tobacco industry directed their advertising campaigns toward a younger audience. Popular and famous role models from the sports and entertainment industries were used nationwide to advertise the products, establishing spit tobacco use as part of a successful athletic and macho lifestyle. This image identification ties it to the adolescent males' need to feel grown up and macho.
"The individual psychosocial variables most closely related to adolescent spit tobacco use include:
1) having friends who use spit tobacco,
2) use of cigarettes and other drugs,
3) parental acceptance of spit tobacco use,
4) willingness to take risks and a desire to stand apart from the crowd."2
Research has shown that of all the factors, peer acceptance, curiosity and tobacco use by family members and close friends are most likely to have the greatest impact on a young person's decision to use spit tobacco. Slightly less impactful variables in choosing to start using tobacco are social image and the belief that spit tobacco is a safe alternative to cigarettes. Ironically, some of the social changes that have contributed to a decrease in cigarette smoking have contributed to the increase in spit tobacco. While smoking is prohibited in most schools, shopping malls, public buildings, and work places, spit tobacco use continues to be tolerated, allowing an addicted smoker to switch to the more convenient tobacco form.
Recent research performed by the CDC has shown that the incidence of spit tobacco use among students nationwide had in fact decreased from 1995-2003; however, the numbers have stayed constant since that time. Continued efforts must be made to decrease these numbers further.
Spit Tobacco in Sports
Of all the sports where spit tobacco can be found, none is more closely associated with the products than baseball. In 1999 it was estimated that 33% to 40% of professional baseball players and 45-55% of college baseball players use spit tobacco. Studies have shown that many players come to Major League Baseball already using spit tobacco. Of the incoming rookie baseball players entering professional baseball, 67% had tried a form of spit tobacco and 31% were current users. Most of them want to quit because of health concerns or for personal and family reasons. Organizations such as NSTEP work closely with professional baseball to provide counseling and support to those players trying to deal with the challenge of quitting spit tobacco use. (http://oralhealthamerica.org/programs/nstep/)
Baseball players have been using spit tobacco since the mid 1800's as a way to help keep their mouths wet on the dusty fields and to relieve boredom. Eventually, it became, in the player's eyes, a traditional part of the game and the culture of baseball. The inherent dangers were not known at the time. During the 1950's, most baseball players smoked cigarettes. As the dangers of smoking were made known, the players, encouraged by cases of free samples, started going back to spit tobacco in the 1970's. In 1990, Major League Baseball issued a report on the dangers of spit tobacco use and started efforts to help players stay off spit tobacco and to educate young players about the dangers of spit tobacco and the difficulty encountered in quitting. "One of the reasons that change seems slow to come in this population is that an attempt is being made to change the social norms of an essentially closed society where spit tobacco use has been commonplace and condoned for many years."3 In 1998, Minor League Baseball extended its ban on the use of spit tobacco throughout all levels of the minor leagues. While not banned in Major League Baseball, progress is being made. The media is cooperating by greatly reducing coverage of actual spit tobacco use during games.
"A national survey found alarming rates of smokeless (spit or chew) tobacco use among male college athletes. In all, 40.0% of college baseball players and 29.0% of college football players had used spit tobacco in the last year. In comparison, the national smokeless tobacco use rate for all college men is 17.0%."4
Since 1994, the National Collegiate Athletic Association, Babe Ruth Leagues and Little Leagues have banned spit tobacco use. This ban includes coaches, officials and athletes in all sports during practice and competition. Most high schools ban tobacco, including spit tobacco, from on campus and campus activities and during games or sanctioned practices held on school property. By having these bans in effect, baseball is trying to send the message that spit tobacco is not part of the culture and does not improve athletic performance. These bans are only effective if there is enforcement. Unfortunately, there are still incidents at all levels where violations by coaches, officials, and players are overlooked.
Baseball is not the only sport where there is a strong spit tobacco presence. There is also a tradition of spit tobacco use in rodeo, car racing, hunting, fishing and golf. Some spit tobacco manufacturers sponsor events in these sports as a way to tie their product and participants of these sports. Music concerts are another type of promotion used by manufacturers to get their message to a younger audience.
Health Effects of Spit Tobacco Use
Chemical Composition of Spit Tobacco
Processed tobacco contains over 3000 known chemical compounds, many of which have been directly linked to causing cancer in humans. There have been at least 28 carcinogenic agents identified in spit tobacco. As of May 15, 2000, The Department of Health and Human Services (DH&HS) added spit tobacco to the official list of "known human carcinogens." According to the DH&HS, cancers of the oral cavity have been associated with the use of chewing tobacco and snuff. Their studies indicate that the tumors often arise at the site of the placement of the tobacco.
The most potent of the carcinogens in spit tobacco are the Nitrosamines, especially N-Nitrosamines, which can be detected in the juice produced from the mixture of tobacco and saliva. These Nitrosamines are formed from the nicotiana alkaloids during the processing of the leaves. The nitrosation process continues in the mouth, stimulated by oral bacteria. The FDA regulates nitrosamines levels in food products; however since tobacco is a nonregulated product, the levels often exceed those found in food by 100-1000 times. Because of the close proximity of the tobacco to the oral mucosal during spit tobacco use, the levels of n-Nitrosamines found in the blood of spit tobacco users are 1.5 to 2.8 times higher than the levels inhaled by persons smoking 20 cigarettes per day.
Other potent carcinogens found in spit tobacco include radioactive polonium 210, benzopyrene, arsenic, cyanide, formaldehyde, cadmium, and uranium. As potent as these carcinogens are, it is impossible to predict when or if cells will become cancerous as a result of continuous exposure. Consequently, spit tobacco users take a risk of developing oral cancer every time they use the product.
Spit tobacco manufacturers add other compounds to their products to achieve the flavors and textures their customers want. Spit tobacco contains high levels of sodium and in many brands, up to 25% sugar and other sweeteners. Flavorings, such as menthol, cherry, and mint, are added to many of the products to make them more palatable.
Nicotine and Addiction
It is no surprise that nicotine, an addictive drug, is a main ingredient in spit tobacco. Nicotine is a plant product and naturally occurs in all tobacco plants. As in other forms of tobacco, spit tobacco delivers nicotine to the user's central nervous system. "It produces transient, dose- related effects dependent on the user's physiology. It acts as a reinforcer, controlling the user's behavior. Tolerance develops with repeated use, with habitual users consuming increasing quantities on a daily basis until a desired level is reached."5 According to the 1988 Surgeon General's Report on Nicotine Addiction, the pharmacological and behavior processes leading to nicotine addiction are similar to heroin and cocaine. As is the case for those other drugs of abuse, nicotine produces effects in the user that are considered desirable to the user.
All drugs of abuse work on the pleasure center of the brain in the same way. The cells in those centers are changed in profound, long lasting ways. These drugs produce common effects on the production of dopamine, a neurotransmitter involved in experiencing pleasure. These effects include transient dose-related changes in mood and feeling. Maintaining desired levels of these feelings is dependent upon continued administration of nicotine. As the level decreases, the user will often experience mood swings, irritability, impulsiveness, anger, and depression. The presence of nicotine in the body also causes skeletal muscle relaxation, cardiovascular effects, and hormonal changes.
Levels of nicotine vary depending on the form and brand of spit tobacco used. According to the CDC, tobacco users who dip or chew 8 to 10 times per day may be receiving the nicotine equivalent of 30 to 40 cigarettes per day. Each dip of snuff contains the same amount of nicotine as 2 to 5 cigarettes. Spit tobacco manufacturers regulate the amount of free nicotine in their product by adjusting the pH of the tobacco. The average pH of tobacco is 7.4, but adding alkaline additives, such as sodium bicarbonate, increases this. Increases in pH will increase the amount and the rate of absorption of free nicotine into the bloodstream.
Studies done by the CDC found the pH level in the most popular spit tobacco brands varied from 5.24 in Hawken® Wintergreen to 8.35 in Kodiak® Wintergreen and Copenhagen® Snuff. Kodiak and Copenhagen are the most popular brands, especially among the habitual users, and also have the highest levels of nicotine and are the most physiologically addictive. They also have the highest concentration of tobacco specific N-nitrosamines.
Spit tobacco users develop a nicotine addiction similar to that of cigarette smokers and have been found to absorb at least as much nicotine as smokers. The rate of absorption from snuff is especially rapid as the high pH of saliva provides a favorable environment for absorption through the oral mucosal. Young users appear to rapidly develop a physical dependence from spit tobacco use and experience withdrawal symptoms after a relatively short period of time as a regular user. The more addicted an adolescent is, the more difficult it will be for them to quit and the more likely they are to become adult users. The Surgeon General's Report of 2012 disclosed that among male high school students, 1 in 10 were current users of spit tobacco. Success rates in spit tobacco cessation attempts by addicted users remain low. In fact, regardless of age, 74% of daily users reported that one of the reasons they continued to use it was because it was hard to quit. Cigarette smokers report it being easier to quit smoking than to stop spit tobacco use.
General Health Consequences
The nicotine in spit tobacco is a poisonous chemical whose use can cause serious health consequences. In addition to its addictive quality, it has been found to activate the sympathetic nervous system resulting in constriction of the blood vessels, reduction of coronary blood flow, and an increased risk of vascular thrombosis. The effects on the cardiovascular system can lead to an increased heart rate (10-20bpm), increased blood pressure (5-10mmHg), and reduced arterial blood flow, causing dizziness, decreased endurance, and stamina. An increase in blood clotting factors may lead to the formation of clots in already constricted vessels, causing a stroke or heart attack.
Studies have shown nicotine to affect the hormonal and metabolic systems. It increases blood glucose levels leading to higher insulin levels and consequential energy swings. The level of the hormone cortisol, involved in wound healing and swelling, is increased by nicotine. This abnormal rise disrupts the normal healing process. Digestive problems have been linked to the nicotine and other chemicals found in tobacco juice. While spit tobacco users attempt to spit out the accumulating tobacco juice and saliva, over 50% of the juice is swallowed. The toxins in the juice cause problems such as acid reflux, esophageal ulcers, peptic ulcers and an increased risk for cancer of the larynx, esophagus, and stomach.
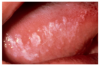
Leukoplakia
"Most moist snuff users place their dip in the same location every time they use it. That site is where 93% of the primary lesions that can lead to cancer, are found."6 These lesions are referred to as leukoplakia and develop in 40-60% of habitual spit tobacco users. Snuff users are 4-6 times more likely to have these lesions than users of other forms of spit tobacco. Risk of having a lesion is increased among a group of users known as "Double Dippers." This group mixes snuff and chew and dips them at the same time, resulting in an increase of negative health effects.
Leukoplakia, also known as a localized epithelial abnormality, can appear after only a few months of regular spit tobacco use. The lesions take several forms, requiring a biopsy for accurate diagnosis. Characteristics include a white color change that cannot be wiped off with gauze, granularity of the surface, wrinkling, corrugation and/or a thickening of the mucous membrane. There may also be red areas intermingled with the white areas and it may be modular in appearance. The frequency and duration of spit tobacco use are positively related to the prevalence of leukoplakia. In heavy, habitual users, over 50% develop oral mucosal abnormalities within 3.3 years of use. The frequency of use (more than 15 minutes at a time for several times a day) and overall length of use are important factors in the likelihood of developing lesions.
Most white lesions will dissipate within 6 weeks after discontinuing tobacco use. Up to 75% will regress if the tobacco is removed from the site. However, it is vital that a patient with a white lesion is re-examined in 2 weeks to be sure that healing is occurring and the tobacco has been removed from the site. If there is no change, a biopsy should be performed immediately. The patient who continues to use tobacco should be taught to do a self-oral cancer screening and to return to his health care professional for regular exams. Not all lesions are discovered before they undergo transformation to a dysplastic state. According to the American Cancer Society (ACS), 3-5% of the leukoplakia are cancerous or exhibit changes that progress to cancer within 10 years if not properly treated.
Oral Cancer
New cases of oral cancer in the year 2013 are estimated at 42,000, resulting in 8,000 deaths. That is roughly 1 death per hour or 24 people every day. The use of alcohol and tobacco is directly linked to 75% of the diagnosed cases. Studies sponsored by the ACS found that using spit tobacco will increase the risk of getting oral cancer 50 times over that of someone that does not use spit tobacco. Historically, oral cancer has been found to be twice as common in men as women. "Of those 42,000 newly diagnosed individuals, only slightly more than half will be alive in 5 years. (Approximately 57%) This is a number which has not significantly improved in decades."
Because oral lesions are often painless and are difficult to detect without an oral cancer screening, they may have been present and growing for many years before producing symptoms such as pain, swelling or bleeding. If the original lesion has spread to surrounding tissue, the surgery required to excise the tumor is extensive and disfiguring and may require the removal of sections of the face, tongue, cheek, lip, or jaw. Subsequent chemotherapy and radiation treatments result in pain, mouth sores, nerve damage, non-functioning salivary glands, dry mouth, decay, and difficulty in swallowing. Depending on the extent of the surgery, oral prostheses may be needed. These prostheses can help return function and esthetics to as close to normal as possible.
The term oral pharyngeal cancer includes cancers of the oral cavity and the pharynx. The most common sites for cancerous lesions to develop are the lateral border of the tongue (20%), gingiva and cheek (18%), floor of the mouth (12%), lips (11%), and the salivary glands (8%). Squamous cell carcinoma is the most common type (90%) and presents as more invasive and with an increased tendency to metastasize than other types. There are several risk factors associated with developing oral and pharyngeal cancer. According to the October 2008 report from the National Institute of Dental and Craniofacial Research (NIDCR), most cases of oral cancer are linked to tobacco, heavy alcohol uses or the use of both tobacco and alcohol together. There are a growing number of cases being diagnosed in people under 50 years old without the historic risk factors of tobacco and alcohol use. Infection with the sexually transmitted human papilloma virus (HPV 16) has been linked to this subset of oral cancers. The risk for cancer of the lips increases with prolonged exposure to ultraviolet radiation. The carcinogenic agents are able to penetrate and damage the DNA in the cells, causing the DNA to malfunction and accumulate abnormal cells resulting in the formation of a cancerous tumor. As the damage increases, the cells will metastasize.
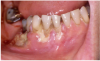
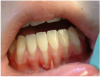
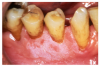
Periodontal Effects of Spit Tobacco
The most notable health consequences associated with spit tobacco use are those seen in the oral cavity. These effects can be recognized by the patient as well as the clinician and provide excellent opportunities to educate the user in the dangers of the tobacco use. Spit tobacco use causes serious short-term health consequences among young people. These consequences include halitosis, staining, abrasion of the teeth, gingivitis, gum recession, dental caries, and tooth loss.
Tooth loss is more common among spit tobacco users than nonusers. This loss is a result of several factors including poor oral hygiene, extensive decay, and destructive periodontitis. Focal gingival recession with periodontal attachment loss and bone erosion occurs frequently on the facial surfaces of the teeth where the tobacco is held. This recession is a result of the irritation caused by the toxic chemicals and abrasives found in spit tobacco. It is not uncommon to find substantial amounts of root surfaces exposed at the tobacco placement site. With the root surface exposed, there is increased risk of hot and cold sensitivity and root decay. While gingivitis may be present, bleeding is less common because of the vasoconstriction properties of nicotine. Instead, the heavy spit tobacco user will likely develop gingival swelling and bleeding as a result of poor oral hygiene.
Additional characteristics of long term spit tobacco use are stained teeth and halitosis. The tobacco and the juice produced can penetrate into the tooth enamel and restorative material, resulting in a brown or yellow darkening of the teeth. These stains, in the presence of poor oral hygiene, can also result in a dark brown line along the gingival margins of the affected teeth. The pitting of tooth surfaces caused by the abrasives in the tobacco results in intrinsic staining. Halitosis is the most commonly recognized negative consequence of spit tobacco use. It is a result of the constant presence of tobacco juice in the user's mouth. In addition, the need to continually spit out excess juice and saliva is offensive and unhygienic. Spit tobacco users often find pieces of tobacco lodged between their teeth, in the buccal folds, and on the lips.
The abrasives found in spit tobacco can also wear away portions of the occlusal/incisal surfaces of the teeth resulting in a weakening and eventual chipping of those surfaces. The abrasives also irritate the gingival tissue, allowing for more efficient absorption of the carcinogenics and nicotine found in the tobacco. As a result of the chemicals and sodium in spit tobacco, users suffer a lessening of their senses of taste and smell. This can lead to unhealthy eating habits. Excess sodium may augment the effect of nicotine on elevating blood pressure.
According to a study conducted by Dr. Scott and Dr. Deborah Winn for the National Institute of Dental Research (NIDR), individuals who use chewing tobacco have significantly more decay on the crowns and roots of their teeth than nonusers. The study showed that men (over 18 years) who use chewing tobacco exclusively were four times more likely than a nonuser to have one or more decayed or filled root surfaces. The more packages chewed, the greater the chance of having decayed or filled surfaces. This increased risk is associated with the high sugar content of the tobacco and the way it is used. Typically a wad of chew is held in the mouth for 30 minutes at a time, and then replaced with a new wad, thus exposing the teeth to the tobacco and sugar for many hours a day.
It has also been observed that spit tobacco users flossed and brushed less frequently than nonusers. Compliance with daily flossing protocol was particularly low. A study performed in 1998 by J. A. Andrews found that even spit tobacco users who perceive that they have serious oral health problems do not compensate for these problems by improving their oral hygiene regimen.
Advertising and Consumption
Released in 2013, The Federal Trade Commission (FTC) Report for the Year 2011 reported that the total amount of spit tobacco sold by manufacturers has gone up from 120.52 million pounds in 2010 to 122.74 million pounds in 2011. The overall revenue for spit tobacco has also gone up from $2.78 billion in 2010 to $2.94 billion in 2011.The overall revenue for spit tobacco has also gone up from $2.78 billion in 2010 to $2.94 billion in 2011.
The FTC Report for the Year 2011 shows expenditures on advertising in 2011 increased from $250.8 million in 2005 to $451.7 million. Spending for magazine and outdoor advertising declined while dollars spent on direct mail, point of sales, price discounts to retailers and wholesalers, free sampling to the public, internet and website advertising, and support for sports and sporting events increased.
A documented strategy, developed by the largest manufacturer of spit tobacco in the United States, to graduate new, young users to stronger brands has been in place since 1984. The strategy has become known as the Graduation Method and has proven to be very successful. Designed to appeal to the very young potential user (10-12 yrs.), a product is marketed as pre-measured packets containing tobacco, sweeteners and flavoring. Designed for the beginner, the packets are sweeter and milder tasting, less likely to cause side effects such as nausea, and are easier to control in the mouth. After a period of time, the young user develops a tolerance to this lower nicotine product and "progresses" to the next level product that supplies more nicotine and a stronger tobacco flavor. Most habitual users will graduate to the strongest snuff with the highest levels of nicotine in order to satisfy their addiction. Once at this level, the user is addicted and would find quitting spit tobacco to be very difficult.
Other techniques used by the spit tobacco industry to attract and keep new customers include coupons and retail value-added promotions, public entertainment, sponsorship of sporting events and concerts, distribution of free samples, magazine advertising, and continuing to use the term "smokeless." Efforts are being made to bring their message of macho images and risk taking to new audiences, such as the Latino community. Links to role models and athletes in the arenas of rodeo, car racing, baseball, football, soccer, fishing, and hunting continue to be promoted by the spit tobacco industry in their appeal to new and younger potential users.
In the last several years, the two largest manufacturers of cigarettes in the United States, R.J. Reynolds and Phillip Morris, entered the spit tobacco market with a new generation of products. R.J. Reynolds is aggressively marketing a variation of snuff under the name of Camel Snus in addition to other products designed to dissolve in the mouth. Phillip Morris has joined this market with Marlboro snus and a marketing plan aimed at all tobacco users with the message that snus is a safer and cleaner than cigarettes.
In 2008, R.J. Reynolds introduced three variations of dissolvable tobacco products (pellets, sticks, and film strips) under the umbrella of Camel Dissolvables. They contain between 60%-300% of nicotine found in cigarettes and are marketed to enable a tobacco user to maintain a tobacco habit in clean indoor air facilities and tobacco free zones. These products were formulated to resemble familiar and socially acceptable products such as tic-tac breath mints, breath freshening strips, and flavored toothpicks.
The dissolvable tobacco products were introduced and marketed in five U.S. cities. After five years, the sales success of the dissolvable products has been limited with surveys showing not only low sales numbers, but a lack of consumer awareness. In August, 2013, R. J. Reynolds announced that they were limiting the distribution and marketing of Camel Dissolvables to two U. S. cities with no plans for expanding the markets. They also announced that they will continue to research and develop new smokeless products.
The Dental Professional's Role in Spit Tobacco Use Prevention
With proper education on the facts about spit tobacco, the dental professional can become a very effective anti-tobacco messenger, in and out of the office. Dental healthcare workers are on the front line of defense when it comes to spit tobacco. They have credibility and empathy with their patients that allow for open communication and trust. The negative effects of spit tobacco on the oral cavity are often very visible to the dental healthcare worker and the patient alike, and provide excellent "teachable moments" while the patient is in the dental chair. The more comfortable the dental healthcare worker is with the danger signs associated with tobacco use, the more effectively he or she will discuss current and future problems with the patient.
Dental Office Protocol
Having an office protocol on tobacco use prevention is very important in order to send a consistent, effective message to the patient. There must be a method to assess the tobacco status of each patient and to record and monitor that status at each visit. The dental healthcare worker can be essential in getting and recording that information. If the patient uses tobacco, the dental healthcare worker can point out existing problems ("teachable moments") and tie them to the tobacco use. It is also important to congratulate patients who have chosen not to use tobacco. When working with children, it is important to present tobacco education in a supportive, non-threatening way in order to help them make the right choice when tempted to try tobacco products.
Community Outreach Programs
There are many ways dental professionals can use their knowledge and skills in spit tobacco use prevention outside of the dental office, including becoming involved with tobacco use prevention groups such as the National Spit Tobacco Education Program (NSTEP) and the American Cancer Society and participate in their community events. The ADAA is involved in a partnership with NSTEP that makes it possible to work through state Dental Assisting societies and local NSTEP coordinators on spit tobacco education projects. NSTEP conducts stadium events at Minor League and Major League Baseball parks and at Little League events and baseball camps for young players. There are many opportunities for a dental assistant to present programs on the dangers of spit tobacco use to youth groups and sports teams, at health fairs and in school classrooms. Brochures, posters, and videos are available for the dental community to use to educate patients, youth, parents, and teachers on the deadly consequences of spit tobacco use. The underlying message to all audiences must be the same: Spit Tobacco use is not a safe alternative to smoking. The dental assistant is in a unique position to spread this message.
Summary
For years spit tobacco has been mistakenly seen as a safer alternative to smoking tobacco. We now know that spit tobacco use can cause many devastating side effects such as increased blood pressure, gingival recession, leukoplakia, as well as oral cancer. Although the statistics have indicated a drop in usage, continued efforts must be made to decrease the numbers further. Dental professionals have a unique opportunity to help their patients understand the inherent dangers of spit tobacco and the available resources to help them quit. The National Spit Tobacco Education Program (NSTEP) and the American Cancer Society have many programs and resources to help patients on the journey to a tobacco free life.
Glossary
abrasion - wearing away of the surfaces of the teeth by friction; excessive wear can be caused by the sand or grit present in spit tobacco
addiction - compulsive use of a habit-forming drug or substance accompanied by increasing frequency and intensity in order to experience the desired effects
carcinogenic - anything that causes cancer
chewing tobacco - tobacco sold as loose-leaf, plugs, bricks, and twists; held in the mouth between the cheek and gums and is chewed or sucked to extract the nicotine
dependence, physiological - condition in which the body relies upon a drug or substance, resulting in specific body cell alterations and a state where continued use is necessary to maintain the body's state of normalcy and balance
dependence, psychological - condition in which the user of a drug considers the effects it produces essential to maintain an optimal state of well being
dipping - act of placing moist snuff in the mouth; dip is considered to be the amount of tobacco held between the thumb and forefinger
drug - substance that can alter mood, perception or consciousness
gingivitis - inflammation of the gingival tissue resulting in redness, swelling, bleeding, and often discomfort
halitosis - unpleasant breath
leukoplakia - formation of white, irregularly shaped, thickened patches in the oral cavity; found at the site of spit tobacco placement; may become squamous cell carcinomas (3%-5% of the cases)
nicotine - an alkaloid derived from tobacco that acts as the addictive agent in both smoking tobacco and spit tobacco
N-nitrosamines - cancer-causing chemicals found in cured tobacco products
oral cancer - cancer of the oral cavity, including the lips, tongue, gingival tissue, hard palate, soft palate, floor of the mouth, roof of the mouth, mucosal membrane, and oropharynx
pH level - degree of alkalinity or acidity of a solution; values above 7 indicate alkalinity and result in a more efficient absorption of free nicotine found in spit tobacco; pH level of tobacco can be regulated by the manufacturer with the use of alkaline additives, such as sodium bicarbonate
plug - chewing tobacco pressed into bricks; firm and moist tobacco
recession - exposure in the roots of the teeth caused by a loss of gingival tissue
smokeless tobacco - tobacco that is not smoked, also known as spit tobacco; term used by the tobacco industry to promote its deadly product as one that is safer than cigarettes
snuff, dry - dry, powdery tobacco product that is usually sniffed into the nose
snuff, moist - finely cut and ground moist tobacco product that is placed in the mouth between the teeth and gingiva or lip. It is also known as "dip"
Surgeon General - chief medical officer of the United States Army, Air Force, or Public Health Service
tolerance - capacity to assimilate a drug, such as nicotine, continuously or in increasing larger doses to achieve a constant effect
twist - dried tobacco leaves that are twisted into ropes and sold in pouches
withdrawal syndrome - intense physiological disturbances that occur when abruptly discontinuing the administration of a drug that, by its prolonged use, induced physical dependence; signs and symptoms include nausea, irritability, insomnia, restlessness, and headache
About the Author
SUSAN C. DODD, RDH, BA
Susan C. Dodd, RDH, BA is the president of SCD Healthcare Consulting, LLC. Prior to starting her consulting company, Sue worked with Oral Health America as Director of the National Spit Tobacco Education Program and as Director of Programs overseeing implantation of programmatic and operational needs for OHA programs, sponsorships and cooperative agreements. She developed and supported state and community oral health coalitions and collaborations and assisted in strategic planning to integrate and coordinate OHA programs and development.
Oral Health America's NSTEP program was a nationally recognized public awareness campaign that in collaboration with the Robert Wood Johnson Foundation worked with public and private sectors to provide tobacco use prevention material and cessation resources, trainings, educational programs and awareness campaigns while working with community partners, baseball organizations, Little League International, professional medical and dental organizations, educators, coaches, parents and children.
Endnotes
1. Severson, H.H. (1993). Nicotine addiction: principles and management. New York: Oxford University Press.
2. Greene, J.C., Walsh, M.M., Legendry, M.A. "Prevalence of spit tobacco use across studies of professional baseball players." CDA Journal, May 1998, 358-364.
3. College Tobacco Prevention Resource. (2002 Mar). College Tobacco Facts: High-Risk Populations. Retrieved January 15, 2014 from the World Wide Web at www.ttac.org/services/college/facts/high-risk.html
4. "The marketing of nicotine by one oral snuff manufacturer." Tobacco Control. Spring, 1995; Vol.4, No. 1.
5. "Smokeless Tobacco Fact Sheet." Connecticut Clearing House; Plainville, CT.
6. Oral Cancer Foundation. (2013) Oral Cancer Facts. Retrieved January 15, 2014 from the World Wide Web at http://www.oralcancerfoundation.org/facts/
References
Andrews, J.A., et.al. (March 1998). "Relationship between tobacco use and self-reported oral hygiene habits." JADA; 129 (3), 313-320.
California Dental Association. "Using smokeless tobacco is gambling with your health." Sacramento, CA; 1998.
Cancer Facts and Figures 2000. American Cancer Society, Inc., 1999.
Centers for Disease Control & Prevention (CDC), "Reasons for tobacco use and symptoms of nicotine withdrawal among adolescents and young adult tobacco users-U.S., 1993," Morbidity & Morality Weekly Report, 21 Oct. 1994, Vol.43, No.41.
CDC. "State Tobacco Highlights-1999," 1999, CDC publication no. 099-5621.
CDC, "Surveillance for selected tobacco use behaviors-U.S., 1990-1994," MMWR, 18 Nov. 1994, Vol. 43, No. SS-03.
CDC. Tobacco Information and Prevention Source. Tobacco Use, Access, and Exposure to Tobacco in Media Among Middle and High School Students - United States, 2004. Available at: http://www.cdc.gov/tobacco/research_data/youth/mmwr_5412highlightd.htm Accessed: April 2005.
CDC. Youth Risk Behavior Surveillance - United States, 2011. CDC Surveillance Summaries2012;61(SS04):1-162
Cooper, J., Ellison, J. A., & Walsh, M. M. (2003). Spit (smokeless)-tobacco use by baseball players entering the professional ranks. Journal of Athletic Training, 38(2), 126-132.
Daughty, Virginia, et.al. (Feb. 1994). "Surveying smokeless tobacco use oral lesions & cessation among high school boys." JADA; 125, 173-180.
Federal Trade Commission, "Report to Congress pursuant to the comprehensive smokeless tobacco health education act of 1986" (1997).
Federal Trade Commission. Smokeless Tobacco Report for the Year 2011. Washington, D.C.: Federal Trade Commission; 2013. Available at: http://www.ftc.gov/sites/default/files/documents/reports/federal-trade-commission-smokeless-tobacco-report-2011/130521smokelesstobaccoreport.pdf Accessed: January 2013.
Grady, D., Greene, J., Daniels, T.E., Ernster, V. L., Robertson, P. B., Hauck, W., Greenspan, D., Greenspan, J., Silverman, S. "Oral mucosal lesions found in smokeless tobacco use." JADA; July 1990; 121.
Klein, J.A., Christen, A.G., Christen, J.A., McDonald, J.L., Guba, C.J. "Understanding nicotine addiction and intervention techniques for the dental professional." ADAA Continuing Education Course: Chicago: 1990.
National Park Service. (1998, February). Tobacco: The early history of a new world crop. Retrieved from http://www.nps.gov/jame/historyculture/tobacco-the-early-history-of-a-new-world-crop.htm
National Spit Tobacco Education Program (2000). [on-line]. Available: http://www.nstep.org
National Spit Tobacco Education Program (NSTEP). (N.D.). Gruen von behren. Retrieved from http://oralhealthamerica.org/wp-content/uploads/Gruen-Von-Behrens.pdf
National Survey on Drug Use and Health, 2002. Tobacco chapter.
"Nicotine varies widely in chewing tobacco." (May 24, 1999). ADA News Daily; ADA; Chicago; 1-2.
"Oral Cancer Causes and Symptoms & The Oral Cancer Exam." National Institute of Dental and Craniofacial Research National Oral Health Information Clearinghouse." NIH Publication, October 2008.
"Oral cavity and oropharyngeal: prevention and risk factors." American Cancer Society. Available: http://www.cancer.org.
"Oral lesions from smokeless tobacco dissipate after stopping use of tobacco products, study concludes." JADA, July. 1999.
Pediatrics, Vol.115; No.3, March 2005, pp 719-725
"Spit tobacco: just the facts!" (1999). Tobacco Control Research Council. National Institute of Health-National Cancer Institute.
"Surgeon General's Report: Preventing Tobacco Use Among Youth and Young Adults." U. S. Dept. of Health and Human Services. 2012.
"The Health Consequences of Using Smokeless Tobacco: A Report of the Advisory Committee to the Surgeon General." U.S. Dept. of Health and Human Services. 1986.
"Tobacco Effects In The Mouth." U.S. Dept. of Health and Human Services. NIH Publication No. 96-3330.
Tobacco Free Utah. (2008, December). History of smokeless tobacco. Retrieved from http://www.tobaccofreeutah.org/pdfs/hissmkls.pdf
U.S. Department of Health and Human Services. National Institutes of Health. Spit Tobacco: a guide to quitting. June 2012.
U.S. Department of Health and Human Services. (2011). National survey on drug use and health:summary of national findings. Retrieved from http://www.samhsa.gov/data/NSDUH/2k11Results/NSDUHresults2011.pdf
Youth Tobacco Surveillance - United States, 2000. Morbidity and Mortality Weekly Report. 50(SS-4): 1-92, November 2, 2001.