You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
The ADAA has an obligation to disseminate knowledge in the field of dentistry. Sponsorship of a continuing education program by the ADAA does not necessarily imply endorsement of a particular philosophy, product, or technique.
Computers and specialized electronic software both are integral parts of any dental practice. The success of any practice rests on the application and implementation of a software that addresses the needs of that dental office. For dental offices transitioning from manual to electronic, it is important to choose a dental software that is specific to the dental team in order to build, enhance and strengthen the practice for years to come.
This course identifies certain functions and concepts in order to facilitate the transition from a manual to electronically based office. There is no ideal software that fits every dental office, but there are principles that can be explored depending on what is desired. The system should function as the central storage facility for all information produced and needed in the office, both now and in the future. As such, a practice's dental computer system must offer the same flexibility that a written record or ledger provides, plus the ability to run reports allowing for more effective management. One important thing to remember is to choose a computer system that is flexible and that can work effectively.
Although this course does not endorse any specific computer system, it presents principles that can be applied to most any digital system.
Implementation: Getting Started
Choosing a Specialized Dental Software Program and Computer System
It is very important that the dental team work together in choosing the best computer system and software that matches the philosophy of the practice and the necessary functions of the practice. The first step is finding an affordable computer system that functions according to the needs of the office and has the capacity to expand to further fulfill its requirements. There are many software companies that cater to dental offices and will perform demos or offer 30-day trials.
Some options to consider:
• Reports - such as financial or production reports
• Scheduling and Patient Recare - for multiple or single doctor practices
• Charting, Treatment Planning and Record Keeping - make sure it is user friendly
• Insurance and Electronic Claims capabilities
Identifying Your Practice Needs
In selecting a dental office computer system, evaluate each option to determine if it can provide the following features:
• Performance and audit reports;
• Dental insurance - plan information and parameters (for example, eligibility, coordination of benefits, estimate of insurance benefits), electronic claims completion and submission;
• Patient accounts - demographics, digital charting and/or paperless charts;
• Scheduling - by room, procedure, or provider;
• Recall/recare and patient confirmation;
• Word processing - charting progress notes, marketing, and referral letters;
• Digital radiographic images, intraoral camera pictures storage and external facial photo storage;
• Accounts receivables - walk-out and account statements, posting patient payments with receipts, full account history, finance charge calculations and tracking payment plans;
• HIPAA compliance - maintaining privacy, transmission security and automatic history backup;
• Accounts payable - payroll, electronic bill paying;
• Inventory control and supply-ordering capabilities;
• Tracking pickup and delivery of laboratory cases;
• Options for email and an office website; however, these may need to be provided by alternate providers.
Available Options
Through advancements in technology, computer software is continuously being enhanced and upgraded. The electronic patient record (chart) allows you to record a patient's health history, periodontal charting, dental charting, and progress notes directly into the practice's computerized database. Four methods of data entry are available:
1. Keyboard and mouse, dental team members enter data at the specified prompts.
2. Voice activation, in which the operator speaks into a microphone and information is automatically recorded by the computer. Some of the earliest models were ineffective, so investigate this thoroughly prior to purchase.
3. Touch pad, through which users enter information by touching letters or graphic images of various teeth, surfaces, and surrounding support structures on a device similar to a keyboard.
4. Pen/Wand, with which users touch images directly on the computer screen.
Hardware Options
Most offices have one computer with a console in each operatory (Table 1). The server, which is interconnected with all other computers in the office, is the central processing unit that stores all programs and back-up memory for the entire practice. It is generally kept in a separate room and all data and functions maintained regularly by the software company. All computers can be accessed by passwords, which are changed often for security measures.
Multiple networked computers consist of several computers interconnected to allow data to be shared and to permit more than one person to access the system simultaneously. This is done by using Ethernet networking cables or by a wireless system and router set up. Ethernet network cables are not commonly used now since wireless systems offer so much more flexibility. Networking all computers in a dental office decentralizes the access and allows for data input at chairside, laboratory, and consultant locations. Significant upgrades to speed and memory needs make it possible for offices to incorporate almost any feature including complete data management and digital radiographs. Digital radiographs often require additional or separate imaging software. Sometimes this photo software is integrated into the digital charting program; sometimes it runs separately but will attach the images into the digital chart.
When using a digital system, do not assume that multiple users may enter information into the patient's chart at the same time. For security purposes and for recording of accurate information, systems usually allow that only ONE person is able to enter data at a time. Others in the office may be able to view the information and the remainder of the patient's chart, however two users will not be able to enter information simultaneously. The data entered must be saved prior to others being able to enter additional information.
As expected with each option, initial start-up costs are considerably less with a single PC system and increase with each additional computer or server installation. Future needs and possible expansion should always be considered before deciding which system is best for the practice setting. Some computer companies may lease office systems and have agreements for upgrades at certain intervals. Consideration as to which option best fits the practice's financial situation should be researched.
Software Support and Upgrades
Reputable dental software companies will include an initial setup as well as hands-on training in all system functions for a specified period of time according to the contract. Additional training and support can be purchased as needed. Always ask if Tech Support covers both hardware and software. Additional support may be required.
Many software programs have automatic updates that are periodically installed and an email or alert is sent as a reminder. Other companies have their Tech Support install and maintain a system in person. Please ask how maintenance of the program and troubleshooting are managed.
Dental Software Functions
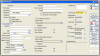
Patient Records Registration Page
All personal information and registration of the patient is entered and kept current. All patient data is kept confidential and updated at every visit. Spelling and correct information is crucial. Such information includes:
• Full legal name, including title (Mr., Mrs., Ms., Sr., or Jr.);
• Billing address;
• At least two telephone numbers;
• Date of birth;
• Emergency contact;
• Current insurance;
• Responsible party;
• Referring dentist;
• Medical alerts.
When entering this information in the computer system, an account number is assigned that represents all pertinent and detailed financial information. Individual patient records then are added and automatically linked with the responsible party's account to keep families together for billing, recall, appointment scheduling, and account retrieval purposes. (Figure 1)
Insurance Coverage Information
To process all claims and thus receive payment from insurance carriers, the following information on insurance coverage is required:
• Carrier information, including the full legal name, address, and telephone number of the insurance carrier;
• Subscriber information, including the full legal name, date of birth, and Social Security number or assigned identification number of the policy holder;
• Employer information for the policyholder, which may include a parent company and its subsidiary (for example, Bakery Union Local 123, Smith's Food Market, Independent School District #833, Park Senior High School) or a single company (such as Jones' Department Store);
• Group name and number information, which is provided by the employer.
• If insurance coverage is not provided by the employer, include all of the policy information provided by the carrier.
Insurance information is applied to all patient members covered under the policyholder's plan, including the patient's date of birth, Social Security number or assigned identification number, and relationship to the policyholder (for example, spouse, child, ward). Primary and secondary coverage may exist for a patient member who is covered by more than one dental plan. As such, it is necessary to determine which of these plans is considered the primary plan and which is secondary. In the case of minors, the birthday rule is frequently used to determine which parent's coverage is primary.
Insurance Plan Information
Some of the most common types of coverage include:
• Fee for Service, also known as "freedom of choice" or "open panel" dental benefits plans. Forms of this type of insurance are Usual and Customary Reimbursement (UCR), Table of Allowances, or Fixed Fee and pay according to plan deductibles and percentages.
• Preferred-Provider Organizations (PPO), these plans establish contracts with participating dentists who agree to discount their fees. Should the patient choose to seek service from a dentist out of contract, the coverage is significantly reduced or eliminated.
• Capitation Programs, which pay contracted dentists a fixed amount, usually on a monthly basis, per enrolled family, or per patient regardless of the extent of treatment.
• Medicaid, a state-funded program in which contracted dentists agree to accept the state's level of reimbursement for services rendered.
A dental computer system should allow information to be customized according to each dental plan's parameters, for example, discounted fees and co-payments.
Patient Information
"Patient information" refers to the details about each family member, including:
• Full legal first and last name, including title (Mr., Mrs., Ms., Dr., Sr., or Jr.);
• Demographic information to include home address, all applicable telephone numbers;
• Full date of birth;
• Social Security Number;
• Gender;
• Responsible party and student status information for minors; and
• Health alert information.
Each family member needs to have an individual patient number. When a new family member is entered into the account, he or she is assigned the next available patient number.
Patient information can be accessed by entering the patient number or through an alphabetical search function by name. (Figure 1)
Account Changes
All software programs allow for changes to patient information. Anything pertaining to patient records can be changed or updated. This includes insurance and charting as well as patient accounts. Many offices have restrictions on who can see certain information; the office manager and dentist can decide on these restrictions.
Recall/Recare
An integral part of any dental practice is its patient recall or recare process. This is the process of notifying the patient of their next appointment for prophylaxis or follow-up care. The office computer system should be able to handle any method of the recall/recare process best suited to the practice. Several systems have an automated phone-dialing feature that speeds the process of calling or texting patients to schedule or confirm recall/recare appointments. Another option is the generation of patient recall/recare postcards. The cost of postage must be considered when opting for this process. There are programs that can generate a postcard that can be mailed to the patient ahead of time.
Scheduling
Computerized appointment scheduling is an asset to the dental practice. Certain parameters can be set, such as:
• Days and hours the office is open;
• Time units for each procedure by provider; and
• Holidays, vacation, staff meeting times and continuing-education days.
These parameters can be easily modified as schedules change.
Automated scheduling functions enable users to search for the first available opening for any restorative or hygiene procedure and to utilize appointment time efficiently by identifying the necessary provider time when using multiple chairs. Once appointment criteria have been entered, the system displays available appointment options. Many systems allow searches for multiple family member appointments on the same day by allowing multiple provider schedules to be viewed on-screen at the same time. Automatic alerts will show for patients that require premedication as their treatment is scheduled.
An enhancement to computerized scheduling is the "Short Call" list, which quickly identifies potential patients who would like to come in sooner if an appointment becomes available.
Posting
Posting is the process of entering treatment data to update patient and account information. This information is obtained from the charge slip or in many updated systems, entered at the chair prior to the dismissal of the patient.
Treatment
As dental procedures are performed, they are entered into the patient's chart along with progress notes. These notes can include, but are not limited to: the date of completed restorative and hygiene procedures, utilized dental materials, home care instructions, consultation notes, and the person entering the information. Each procedure has a specific code designated by the ADA for insurance purposes, which makes data entry easier and efficient. As information is entered, it is automatically saved and cannot be altered unless the provider of treatment overrides the entry. Amendments can be entered at a later time if an entry is found to lack information or be in error. This is usually only available when the provider of service logs on and makes necessary changes. It can be altered by certain staff and modifying the note with another revised notation. Nothing is erased, and anything can be traced to the original author.
Codes
The Code on Dental Procedures and Nomenclature (CDT Code) is a HIPAA designated standard code set. Its purpose is to achieve uniformity, consistency and specificity in accurately documenting dental treatment. It is used to provide efficient processing of dental claims and to populate an Electronic Health Record.
As a named HIPAA standard code set, any claim submitted on a HIPAA standard electronic dental claim must use the dental procedure codes from the version of the CDT Code in effect on the date of service. The CDT Code is used on all paper dental claims, and the ADA's paper claim form data consent reflects the HIPAA electronic standard.
It is becoming more common for the treatment, ADA/CDT code, fees charged and any treatment notes to be entered chairside prior to the dismissal of the patient. Once this occurs, the Auxilliary dismissing the patient can escort the patient to the front desk team members where they are able to see the procedures and charges entered, financial arrangements can be made, as well as the next appointment as requested by the doctor.
Charges
When posting charges, access the individual patient number and enter treatment codes. The software displays the written description and the fee. If tooth numbers and surfaces are applicable to the procedure, the system prompts the user for this data. If the code does not require such information, the cursor automatically bypasses these fields. Multiple charges can be entered for each visit. Upon completion, the information entered is linked to the family account.
For variable-fee procedures, the system allows overriding of the standard charge. For example, denture repair cost may be determined by laboratory fees. Changing a fee in an individual account does not affect the fee stored in the code file. Always check with the doctor regarding fees.
The system keeps track of charges generated by each provider. It asks for the "Provider Number," and users enter the number assigned to the doctor, assistant, or hygienist who provided the services.
Many systems have a "calculator" on the screen to show the previous balance, new charges, and new balance. This simplifies requests for payment at the time of the patient visit.
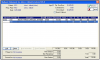
Some systems can print an up-to-date walkout statement. The walk-out statement can be given to the patient along with a reply envelope to help reduce the number of monthly billing statements that must be mailed. (Figure 2)
Accounts Receivable
The dental team member, often the business assistant, must enter the correct payment code (for example, cash, check, insurance, credit card, money order). In response, the system displays the description of this code. Follow up by entering the amount of the payment in the format required by your system (e.g., "$10.00," "10.00," or simply "10").
The front desk should enter in the correct information into the Account page with special attention to detail. Making a mistake on the fees and service codes can sometimes cause multiple problems for the dentist by delaying the reimbursements or insurance audit of the office.
Adjustments
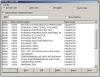
As applicable, the correct adjustment code is entered for any insurance adjustments and discounts (the system displays the written description for the code), and then the dollar amount of the adjustment is entered. The code determines whether the adjustment is treated like a charge (increasing the balance) or a payment (decreasing the balance). The system automatically adds or subtracts this amount from the account balance. (Figure 3)
Transaction Changes
All charge, payment, and adjustment entries must be checked for accuracy. It is necessary to verify all information at the time of entry and generate a Daily Journal Report or Provider Daily Summary from the system. Most systems do not allow changes to any posting after the posting has been saved and approved by the provider. If an error is found after that time, it must be corrected through adjusting entries. Protocol must exist if a transaction requires amendment to maintain information integrity.
Insurance Processing
To process an insurance claim, it is necessary that the document include patient demographics, subscriber information, and coverage data pulled from the account information screen as well as the charges and codes that have been entered through the posting function.
When treatments are posted to a patient account with insurance coverage, the system asks if it should create an insurance claim. It also should be able to coordinate benefits between primary and secondary carriers, as well as apply the birthday rule.
Each time charges are posted, the system should offer the option of printing a claim or saving it for later batch submission. Claims can be produced for either completed treatment or pretreatment estimates. Some systems permit notes for unusual services at the time of posting.
Claim Requirements
Claim requirements are determined by the fields on the standard ADA Insurance Claim Form. The field information is pulled from a combination of files, so if any account, patient, or insurance information is missing or inaccurate, the resulting claim form is incomplete, and payment could be denied or delayed.
Submitting Claims
After an insurance claim has been printed, it is reviewed to determine whether attachments (for example, x-rays, periodontal probing documentation, or other specific documentation) are needed. When claims are computer-generated, the patient may not always be available to sign the claim form, so a signature on file is commonly used. To ensure that signatures are available for all insurance forms, the patient is instructed to sign a Release of Information and an Assignment of Benefits form as part of the patient registration form. When the claim is prepared, the computer prints "Signature on File" and "Assignment of Benefits in the appropriate boxes."
Electronic Claims
Not all claims are submitted on paper. Claims may be sent electronically from the office computer to the carrier's computer. Some insurance carriers choose to utilize a clearinghouse, such as the National Electronic Information Corporation (NEIC), or have developed their own online capabilities. Claims data then are automatically transferred, and no paper claim form is required. Because there are no signatures on an electronic claim, the office must have the patient's signature on file to submit insurance claims electronically in order for the third-party payor to reimburse the provider. By submitting a claim electronically, turnaround time for receiving payment is reduced.
Resubmitting Claims
Manually tracking insurance claims can be very time consuming. Many computer software programs have insurance audit reports that allow users to specify unpaid claims for 30, 60, or 90+ days past due. With this information, claims can easily be reprinted or electronically resubmitted for payment.
Pretreatment Estimates
A pretreatment estimate calculates planned treatment; that is, treatment not yet provided. Certain types of treatment, such as crowns or denture work is often sent for pre-determination for the benefit of both the office and patient. The response from the insurance company states the eligibility of treatment and the percentage of payment from the third-party payor as well as the patient.
The procedure for preparing a pretreatment estimate is slightly different. The system asks questions similar to those found in posting charges, and the same charge codes are used. However, there are two major differences in creating and obtaining pretreatment estimates:
1. These charges are not posted to the patient's account, and
2. The claim form does not show a date of treatment.
Billing
The billing function can be set to generate statements monthly or on a cyclical basis. These statements can be produced using a laser or inkjet printer with a great variety of preprinted forms. In addition to monthly or cyclical billing, most systems can automatically create walk-out statements from account postings. Walk-out statements show the itemized charges and payments for the day or for a range of dates. Some systems allow the patient to choose the billing date (from the first to the 28th of the month), which may be helpful in cases with an established financial arrangement for orthodontic work, an extensive treatment plan, or an overdue balance to be collected over time. If financial arrangement payments are overdue, a regular statement may be generated. Printing options include alphabetical, by ZIP code order, by account number, by individual doctor, or for all doctors in the practice.
Finance Charges
The software also may offer the option of adding a finance charge on overdue accounts. As part of the system parameters, the individual practice establishes how much is charged and when the charges begin to appear (for example, when the account is 30, 60, 90, or 120 days overdue).
Statements and Cycles
A computer-generated statement includes an age analysis of the account balance. That is, it shows the total as well as how much of the balance is current, 30, 60, 90, or 120 days overdue. Most systems require that monthly aging be performed before statements are printed. This step must be carried out, or the records will not be correct.
For practices that add a finance charge to overdue accounts, a system parameter allows the user to determine at what point it begins charging interest (for example, when the account is 30, 60, 90, or 120 days overdue) and at what percentage rate the interest is calculated.
The monthly statement first shows a balance-forward amount for any unpaid charges. It then itemizes all account activity since the last statement. If the system has insurance estimation capability, the estimated insurance payment is printed, as well as any financial arrangements.
The statement also prints any personalized comments that users may have added and designated to print. Statements are printed using preprinted office forms and usually sent with a return envelope. (Figure 4)
Past-Due Notices
The dental software will include a method of notifying the patient of a past-due balance. It may be through a message printed directly on the monthly statement or in a series of letters, depending on the delinquency of the account. Each notice uses stronger terminology with respect to the age of the account balance.
Word Processing
The system will allow users to perform word-processing functions. With a word-processing feature, dental team members can create personalized, professional marketing flyers, referral, and thank-you letters as well as other correspondence. It also allows users to efficiently handle inter- and intra-office correspondence and memos.
Management Reports
Information compiled in Management Reports is customarily available only to the dentist(s), practice manager, and accountant. As they are generated, they are used to analyze the practice according to production by procedure, date, or provider along with actual and estimated revenue and profit reports. These results can be shared with the team to show specifically how and where the practice can improve and grow.
Security Access
Because some management reports contain sensitive data, the system requires a security code as a safeguard. With this feature, the correct security code must be entered before such reports can be accessed. Without the correct code, the system does not allow a user to progress any further. This feature protects private information such as tax and payroll reports, and private health information.
Accounts Payable
Dental practice software is most often included or may be purchased separately to allow users to totally computerize the dental practice. Records of payments to various vendors, including dental laboratories and suppliers, as well as other practice expenses (patient credits, rent, utilities, etc.) can be easily tracked and balanced using this feature. This same option allows check writing, printing, and updating of the check register via the office computer system.
Payroll
Most dental software has a built-in payroll program or the ability to use an online payroll processing company. Some systems contain an option that time stamps employee hours from sign in to sign out eliminating the need for a manual time clock or time sheet.
Daily Journal
The computerized Daily Journal report is similar to a pegboard daily journal page, except that the math calculations are done automatically. As with a calculator, the system can only work with the data it has been given, so it is important that the entries be accurate.
The report is to be printed daily and checked against the charge slips and payments received to be certain that all posts have been entered correctly. Some systems also cross-reference the schedules to ensure that all patients' procedures have been posted and no transactions are missing.
Audit Trail
A comprehensive computer system provides an Audit Trail report. A companion report to the Daily Journal, the Audit Trail shows all deleted transactions. Maintain the audit trail as a record of all deleted transactions to ensure against errors and possible embezzlement.
Deposits
Daily bank deposits of all posted payments must be made to a financial institution to maintain continuity with the Daily Journal and Audit reports. A deposit report will confirm all cash, checks, credit card payments paid to the practice for services rendered. The monetary deposit receipt must match the figures reported by the computerized system. If the balances do no match, further research and correction(s) must be completed. The final corrected report is then regenerated and saved into the permanent record.
Accounts Receivable
The Accounts Receivable report shows all balances by account with breakdowns as to how much is current and how much is overdue by 30, 60, 90, or 120 days.
Dental computer systems should allow users to select a wide range of criteria and provide flexibility in generating an aged receivable report (for example, "choose all" or a select specific monthly aging balance, "include financial arrangements," and "include comments" created after a specific date (Figure 5).
Delinquent Accounts
The Delinquent Accounts report can be used to follow up on overdue accounts. The report shows account name, aged balance, date of last payment (personal or insurance), pertinent telephone numbers, and any financial arrangements that have been made. This report is generated by amount (for example, all balances over $50) and age (such as "all accounts over 60 days past due"). In order to be used effectively within the office's accounts receivables reports, the system should have additional management reports that allow users to track and follow up on unfiled and unpaid insurance claims.
Information Protection and Management Back Up
Daily backup of data is a very important system management function. The computer stores all of its records on electronic media and thus requires the protection of being "backed up" (duplicated and stored elsewhere) to guard against corruption or other loss of data. Since the data in the system changes daily, backup should be part of the office's daily routine, usually at the end of each business day. These files should be stored outside of the office in case of fire or other disaster. While this is still one method for backup, the more modern method is to subscribe to a service for backing up data. These services utilize the Internet to provide continuous backup of data throughout the workday and store dental office data off-site. This eliminates the need to have employees perform the backup, take digit devices off-site for storage or have to retrieve and bring devices back on-site whenever disaster recovery efforts are required.
Archiving and Purging Information
Patient records must be maintained for a certain amount of years according to state's laws. Dental software programs offer the ability to archive inactive patient and office records. The system should also allow for basic purging of data. Purging is the process of "offloading" information (financial as well as treatment) that is no longer required to be legally maintained. The practice needs to determine how long to maintain practice records according to their state's laws. Stockpiles of outdated information can slow the computer's processing time.
Virus and Adware Protection
Offices that utilize the Internet for research, inventory control, and connectivity with other dental offices must load additional software to protect against computer viruses and malware. Should the system be infected, it must be shut down until cleaned. During this time, manual appointment scheduling and financial postings would be utilized to maintain office operations.
Health Insurance Portability and Accountability Act (HIPAA)
The Health Insurance Portability and Accountability Act is better known by its acronym - HIPAA. HIPAA rules and regulations apply to health care providers, including dentists who submit claims electronically, health plans, and health care clearinghouses for which the U.S. Department of Health and Human Services (DHHS) has established a standard, either directly or through a vendor or clearinghouse. Among other purposes, this 1996 Act is intended to improve portability and continuity of health insurance coverage in the group and individual markets; to maintain patient privacy; to combat waste, fraud, and abuse in health insurance and health care delivery; to promote the use of medical saving accounts; to improve access to long-term care services and coverage; and to simplify the administration of health insurance.
Computerized software programs will always be updated to cover the office's HIPAA regulations. Just as with paper driven offices, HIPAA laws about sending electronic information to another entity must be followed or fines can be charged per incident.
The intent of HIPAA is to protect patient privacy and provide security of health records without impeding patient care. When treating a minor, HIPAA defers to state law in determining who serves as the minor's "personal representative." Health care providers may disclose patient health information to persons responsible for payment, as long as disclosures are limited to information needed to obtain payment.
Patients have a right to inspect and have copies of their records. Exceptions include psychotherapy notes, certain records maintained by laboratories, and additional information compiled for legal proceedings. A reasonable, cost-based fee may be charged for this service. (Consult state legislation, as state privacy laws may specifically define this cost.)
Dental team members must familiarize themselves with state privacy regulations. Federal HIPAA privacy and security regulations usually preempt state law, unless state laws require greater patient protection than HIPAA.
Summary
When it comes to computerizing the dental office, research concerning software use and employee training must be considered. Selection of a system that will grow with the practice is recommended. Identification of practice needs for now and for the future, options and software support and staff training are additional concerns.
Computerization of the dental office should fulfill primary needs: It should effectively control and manage information and patient time. More importantly, it should enhance every facet of office communications, improve efficiency, and help the dental team to maintain a higher level of organization. The right system can give team members more time to focus on patients while receiving care and the check-out process-a detail that communicates to patients how important they are to the practice.
Glossary
Account Number - The number assigned to access information on the responsible party, member information, and insurance data.
Accounts Payable - The record of all expenses owed by the dental office.
Accounts Receivable - The outstanding balance on all patient accounts; all money owed to the practice for patient services (usually reported by account, showing both the total balance due and a breakdown of the account age).
ADA Insurance Claim Form - A standard form developed by the American Dental Association that outlines the information needed to submit claims to most insurance companies.
ADA Procedure Codes/Current Dental Terminology Codes (CDT) - A system of numeric codes developed by the American Dental Association for insurance-reporting purposes.
Adjustment Code - The code used to increase or decrease an account balance.
Aging - An internal function whereby the system automatically "ages" all account balances into a period of delinquency, for example, 30, 60, 90, or 120 days past due.
Audit Trail - A record of all entries and transactions that have been deleted or changed.
Backup - Copies of data files kept as a safeguard against damage or loss.
Birthday Rule - Used to determine primary and secondary insurance coverage for dependents. The rule states that the parent or guardian whose birthdate, by month and day only, falls earliest in the calendar year is determined to be the primary provider.
Character - Every letter, number, punctuation mark, or space input to a computer system.
Credit - An accounting entry of payment or adjustment that reduces the account balance.
Cursor - A blinking indicator on the computer screen that indicates the position of the next character to be entered by the operator.
Data - Information that can be organized/analyzed by the computer.
Database - A collection of data or related files arranged for easy retrieval by the computer.
Debit - An accounting entry that increases the account balance.
Default - An assumed or "standard" value used by the system.
Electronic Claims Transaction - The paperless submission of insurance claims, in which data is transferred via modem from the practice computer to the insurance carrier's computer.
Ergonomics - The science of fitting the workplace to the employee. Adjustments made to placement of objects and equipment can reduce workplace stress injuries and possible work-related musculoskeletal disorders (WMSD).
Field - The area on the computer screen in which specific information is requested, for example, name, address, city, state, ZIP code.
Function - A task, such as "Posting" or "Printing Insurance," that is identified on the menu.
HIPAA - Health Insurance Portability and Accountability Act of 1996.
Insurance Carrier - The company that administers dental benefits for a given employer group.
Internal Coding - Codes established by the individual dental practice that allow more flexibility when entering information (when printing insurance claims and similar records, the system automatically converts these into the applicable ADA procedure code.)
Menu - A display that enables the operator to select the desired function.
Modem - Used to transmit data from one computer to another, a device that couples a computer terminal with a telephone line or cable system to connect us to the Internet.
Networking - Tying together several personal computers with one server that holds the database.
OSHA - Occupational Safety and Health Administration.
Patient Number - The number assigned to an individual patient who is a member on a family account.
Payment Code - The type of payment applied to an account balance, for example, cash, check, money order or insurance check.
Personal Computer - A single-user computer with its own processing functions and database.
Posting - Entering transaction data into the financial bookkeeping system.
Pretreatment Estimate - The process by which a patient's treatment plan is sent to the appropriate insurance company on an insurance claim form to obtain prior approximation of insurance benefits.
Privacy Rule - (as it relates to electronic patient information) A component of HIPAA requiring dental offices to implement the necessary physical, visual and technical safeguards to protect patient information.
Prompts - Messages to help users enter appropriate information in the proper format; also known as "helps."
Provider - A professional within the practice, such as a dentist, who provides patient care that, for accounting purposes, is "credited" to that professional; also can be a dental hygienist or expanded functions assistant for patient treatment purposes.
Purging - The process by which data are eliminated and cleared from a database.
Responsible Party - The person obliged to seeing that the account is paid.
Screen - The medium used to review data being entered into and received from a system; commonly referred to as the monitor.
Security Rule - HIPAA component that defines highly detailed standards for the integrity, availability, and confidentiality of electronic protected health information and addresses both external and internal security issues with administrative, physical, and technical safeguards. Standards change periodically and are governed by the Department of Homeland Security.
Server - A computer or computer program which manages access to a centralized resource or service in a network. Servers can provide various functionalities, often called services, such as sharing data or resources among mulitple clients, or performing computation for a client. A single server can serve multiple clients, or a single client can have multiple servers. Typical servers are database servers, file servers, mail servers, print servers, web servers, game servers, and application servers.
Signature on File - The patient's signature on a "Release of Information" and an "Assignment of Benefits" form (instead of having the patient sign each insurance claim form, these signatures serve as proof of the patient's authorization).
Transaction - Each charge, payment, or adjustment posted to a patient's account.
User - The person entering data into the computer system.
WMSD - Work-related musculoskeletal disorders can occur if someone is causing stress and strain to their body due to extended improper posture, repetition and force of movement, over-reaching, and dim or overly bright lighting.
References
ADA. A Guide for Employers: Managed Care, Selecting a Dental Benefits Plan. Chicago: ADA, 1995. ADA. HIPAA 20 Questions: Answers to Your Inquires About the Privacy Regulation; ADA Legal Advisor, April 2003. Available at http://www.ada.org/members/resources/pubs/adviser/0304/adviser_02.asp Accessed June 2003.
Bird D. and Robinson D., Modern Dental Assisting, 9th Ed., Saunders, 2009
Holoway, Toth, Wolfe. Coordination of Benefits Handbook. Thompson Publishing Group, 1992;
Sudimack LE. Insights on Finding a Computer for the Growing Dental Practice. Dental Economics, December 1988
Sudimack LE. The Windfalls of Computerization. Dental Economics, April 1987
About the Authors
Connie Effinger, BS
Connie Effinger has extensive dental operations management experience dating back to 1974. Her skills include computer system setup, training, and support.
Suzanne Kump, MBA, CDA, LDA
Suzanne Kump has been a dental assistant since 1978. Her areas of expertise include chairside skills, orthodontics, and practice management. She has had experience with several computerized dental systems.
Kathy Zwieg, CDA, LDA
Kathy Zwieg has been employed in numerous roles in dentistry, including clinical, practice management, director of operations, and dental assisting program instructor. Besides her involvement in computer demonstration, training, installation, and setup, she has had experience with several dental software systems.
Wilhemina R. Leeuw, MS, CDA
Wilhemina R. Leeuw is a Clinical Assistant Professor of Dental Education at Indiana University Purdue University, Fort Wayne. A DANB Certified Dental Assistant since 1985, she worked in private practice over twelve years before beginning her teaching career in the Dental Assisting Program at IPFW. She is very active in her local and Indiana state dental assisting organizations. Prof. Leeuw's educational background includes dental assisting both in clinical and office management capacities, and she received her Master's degree in Organizational Leadership and Supervision.
Reviewed and Revised by
Christine Casile, CDA, RDA, RDH
Christine Casile is a Faculty Professor at the School of Health Professions (SHRP) - Rutgers University Department of Allied Dental Education. She received her Bachelor of Arts in biology from Drew University in Madison, NJ and is completing her Master's in Healthcare Education at Rutgers University.
Mary T. Elliott, RDA, CDA, EFDA, EFODA, BS
Mary began her professional life earlier than most healthcare providers as her father was a physician. Working in his practice as a Medical Assistant on Saturdays, during the summer and through college was just part of growing up. After high school, Mary began her studies in Nursing. From there, she decided to try dentistry to experience another aspect of the healthcare arena and loved it! She graduated from the University of Oregon's Dental Radiology Program in 1974 and went on to secure her "Certified Dental Assistant" credential from DANB, her "Expanded Functions" license in Oregon, her "Registered Dental Assistant" license in California, her "Registered Dental Assistant" certificate in Washington, a Bachelor of Science degree in "Healthcare Administration" from Concordia University and passed the Western Regional Board Exam in 2014 to place restorations.
In addition to practicing dentistry, Mary has been teaching since 1985 and currently serves as a medical and dental faculty instructor for a variety of colleges in Portland, OR. She also utilizes her dental skills in volunteer clinics providing care to those in need and serves the American Red Cross part time by teaching courses in Disease Transmission, Basic Life Support, CPR, etc.
Mary stays active in the local dental community, assists schools and the ADAA with curriculum revisions upon request, and remains an approved instructor by the Oregon State Dental Board.