You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Local Anesthesia in Today’s Dental Practice
INTRODUCTION
Local anesthesia is the mainstay of modern dental practice, with patients demanding better and more painless dental procedures. Even though local anes-thesia was introduced to the dental profession more than one hundred years ago, today’s options for anesthetizing specific sites in the mouth have become more varied, with dental professionals having many more options to ensure the comfort and safety of their patients. Today’s local anesthetics employ a cartridge, needle and syringe. The syringe is reuseable, while the cartridge and needle are single use. Because an estimated 300 million anesthetic cartridges are used each year, it is critical to have a broad knowledge of the wide variety of products available, correct techniques for using them, and how to manage reactions or emergency situations.
Dental auxiliaries have an important role in assuring the comfort and safety of dental patients before and after administration of local anesthesia to patients within a dental practice. This course is intended to provide dental professionals with basic knowledge on local anesthesia.
HISTORY OF LOCAL ANESTHESIA
For over a hundred years, local anesthetics have been used for dental procedures. Although dentists first introduced anesthesia to the world, it was a physician who used the first local anesthetic for a dental procedure. Local anesthesia has been making life more comfortable for dental patients since 1884, when William Halsted, MD, used a local injection of cocaine to perform the first peripheral nerve block. Even today, dental schools across the country teach a variation of Dr. Halsted’s mandibular nerve block.
The most successful local anesthetic used in dentistry, procaine, was introduced in 1904 by Alfred Einhorn. The drug’s brand name, Novocain®, was once recognized by everyone. Today’s dental professionals have many options to choose (see Table 1). During World War I, Dr. Harvey Cook, who had observed brass munitions cartridges, created the first anesthetic cartridge for dentistry using brass cartridges and pencil erasers as stoppers.
About 40 years after the introduction of procaine, Dr. Niels Jorgensen developed a procedure now known as intravenous conscious sedation. Dr. Jorgensen used intravenous injection, which he called “intravenous premedication," to administer a combination of pentobarbital, meperidine, and scopolamine. Since 1955 his technique has been accepted as an adjunct to local anesthesia, taught as early as 1945 in the Loma Linda Dental School. In 1948, a new local anesthetic, lidocaine, was introduced by Nils Lofgren of Astra Pharmaceuticals. This has become the “gold standard" for local anesthetics in dentistry.. Beginning in 1972, the American Dental Association’s (ADA) Council on Dental Education published “Guidelines for Teaching the Comprehensive Control of Pain and Anxiety in Dentistry." These guidelines were first published in the Journal of Dental Education and are continually updated as needed by the ADA House of Delegates.2
PURPOSE AND TYPES OF LOCAL ANESTHESIA
Reduced pain and anxiety is the purpose of using local anesthesia during dental procedures. Local anesthesia is produced by the application or injection of a pharmacologic agent to eliminate pain or sensation in a specific area in the mouth for a short period of time. These agents are commonly used for most dental procedures to ensure patient comfort and safety, based on the professional judgment of the dentist.
Cocaine, which comes from the coca bush, is the only naturally occurring anesthetic agent, but cocaine has not been used in dentistry since the early 1900s. All local anesthetics currently in use are synthetic.3 Generally, local anesthetics contain the active ingredient and a vasoconstrictor, such as epinephrine. There are other vasoconstrictors available such as Levonordefrin® when reduced dosages of epinephrine are recommended.
For anesthetic cartridges, colored bands can provide an added check on the type of anesthetic being used. The following color code format for banding of cartridges is used for various local anesthetics with varying amounts of epinephrine. Many dentists or hygienists may use more than one type of anesthetic when working on different areas of the mouth. It is important for the dental professional to be aware of the color bands on anesthetics as a check on the product that is being requested in the syringe.
•The color code shall consist of a band 3.0 ± 0.5 mm wide at a distance of 15 ± 5 mm from the stopper end of the cartridge.
•The end cap of the cartridge may be either color-coded to match the ADA Color-Coding System or given a neutral color.
•The stopper will not be color-coded and should not be indicative of the drug or color code.
•Lettering on the cartridge shall be black and font size should follow FDA labeling guidelines (headings at least 8 point type and text at least 6 point type).
•Lettering shall be in durable print that will not be removed by normal office handling.
Topical Anesthetics
The goal for using topical anesthetics is to reduce discomfort associated with an injection. A topical anesthetic is applied to numb the surface of the gingiva in preparation for injecting a local anesthetic at that site.
Unlike injectable anesthesia, topicals anesthetize only the top portion of the mucous membrane or tissue and do not provide anesthesia for the teeth or bony structures. They are used to anesthetize the surface of an injection site. Most topical anesthetics require up to a minute to anesthetize the area, thus, always check the manufacturer’s directions for use. Whenever possible, use topical anesthetics to minimize the patient’s pain associated with injections. For example, after the tissue is dried, a topical anesthetic can be applied to a sterile cotton swab and placed at the injection site prior to the actual injection. It is important to use a topical anesthetic for maxillary lingual injections, just medial to the first molar, because these can be among the most painful sites for injection.
A variety of topical anesthesia agents are available, including lidocaine. In recent years, oral cavity patches have been developed that adhere to the gingiva and deliver targeted, consistent release of topical anesthesia. These have been found to provide more effective pain relief than topical applied with a swab, when using large needles that are inserted to the bone.
Injectable Anesthetics
Local anesthetics are classified into two general categories according to linkages: amide (NHCO) linkage and ester (COO) linkage. These specialized linkages join to a common carbon chain that is joined to a hydrophilic chain of amino (which confers the pKa of the anesthetic). Most injectable anesthetics are amides.4 All local anesthetics that are available in cartridges have pKas that range from 7.7 for Mepivacaine to 8.1 for Bupivacaine, thus making them weak bases. Procaine is the prototype for esters, although it is no longer available in dental syringe cartridge form.5
Table 1 summarizes some commonly used local anesthetics and Table 2 notes the color band used by different products, according to the American Dental Association. Absorption of the pharmacologic agent is dependent on a number of factors, including whether the pH of the tissue has dropped due to localized infection. Other factors include drug solubility, vascularity of the tissue at the injection site, and the impact of the agent on circulation. As such, duration is highly variable and specific for each drug. (Refer to the current Physician's Desk Reference — or “PDR" — for duration and potential side effects of specific products.)
Onset of anesthetic action and duration are affected by a number of factors. The most significant among these appears to be the pH, which drops when infection is present. A product, Onset®, is available that is used to adjust the pH of the anesthetic to match the pH of the tissue so that it is more likely to be effective. Other factors include the pKa of the anesthetics, the % of active ingredient of the drug, the amount of vasoconstrictor present, and the injection technique relative to nerve morphology. Use of vasoconstrictors, such as epinephrine, ensures that anesthetic is not diffused from the injection site. One key factor that is important to reinforce is that injection into a blood vessel is contraindicated. When epinephrine is injected into a blood vessel syncope (see neurotoxicity) can occur; therefore, aspiration prior to injection of local anesthesia into tissues is critical.
Noninjectable Anesthetics
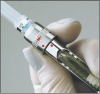
Non-injectable local anesthetics are a more recent development in dental anesthesiology. U.S. Food and Drug Administration (FDA) approved for use in adults who need localized anesthesia in periodontal pockets during scaling or root planing. Oraqix® (a lidocaine and prilocaine periodontal gel) is packaged into single-use cartridges and applied directly into the pocket with a blunt-tip applicator and its specially designed dispenser (Figure 2); it is not for injection. With a 2-minute onset and 20-minute duration, it can be applied to one or more periodontal pockets simultaneously. It can be reapplied as needed up to the maximum dosage of five full cartridges at one appointment.6
ADMINISTRATION OF ANESTHESIA
Dentists are licensed to administer anesthesia, and many U.S. states and the District of Columbia allow dental hygienists to administer local anesthesia under the supervision of a dentist (Figure 3). State education requirements vary for accreditation or board certification in the administration of local anesthetics by dental hygienists. Since requirements change and are different from state to state, check with your state dental practice act for the most up-to-date information.
ROLES OF THE DENTAL ASSISTANT
Although at the time of this publication no state allows dental assistants to deliver anesthetic injections, dental assistants nonetheless are an intricate part of safe delivery of local anesthesia. Dental auxiliaries assemble and prepare syringes, transfer syringes to other dental professionals and often disassemble syringes. Safe handling of used needles is a critical role for dental assistants to avoid needlestick and other sharps injuries.
Accuracy of the Medical History
The patient’s medical history must be complete and up-to-date. Patients should provide a complete medical history, including information on current and past health conditions—especially liver and kidney functions, as these organs are important in clearing local anesthesia from the body. The medical history should list all medications the patient is taking and document whether the patient uses any recreational drugs. The dentist should know if the patient is taking any drug, prescribed or otherwise, that may affect the use of local anesthesia. Examples of such drugs are tricyclic antidepressants, such as amitriptyline (Elavil®); beta blockers, such as propanolol (Inderol®); recent surgeries or general anesthetics, such as halothane (Fluothane®);5 and illicit drugs, such as cocaine. Finally, be sure the medical history notes any past allergic reactions.
Many dental practices post a copy of their medical history forms on their websites so patients can download them and fill them out in advance. Examples can be found at:
http://www.prehndental.com/forms/Form_PATIENT_MEDICAL_HISTORY.pdf
http://www.dentalgentlecare.com/medical_history.htm
Some practices even post medical history forms in Spanish:
http://www.steppingstonestosuccess.com/products/c113lsp.pdf
Even with an initial medical history completed and on file, always question returning patients at each visit to ensure that any changes are noted. It is helpful to prompt them with specific questions about any new medications or recently diagnosed allergies or medical conditions.
Informed Consent
Dental auxiliaries also play a role in obtaining informed consent from patients undergoing dental procedures, including the administration of local anesthesia. Consent must be obtained in writing before any anesthetic is administered. Patients who are minors (e.g. under 18 years of age) or patients who by state law have legal guardians or authorized medical authorities cannot legally give consent. This includes, but is not limited to patients who are not mentally competent to understand any risks associated with the procedures. This can also include patients with developmental delays or dementia. In these situations consent must be given by a parent, other family member, or court-appointed guardian. Resolve consent issues at a preoperative appointment, whenever possible.
Patient Monitoring
Dental auxiliaries are involved in monitoring the patient throughout the dental procedure. During the actual injection the auxiliary should be positioned to block the patient’s arms and hands should the patient reach for the dentist’s hand. In addition to ensuring that the patient is as comfortable as possible, auxiliaries should continually observe the patient after anesthesia is delivered to ensure that the patient is not in distress or developing an allergic reaction. Signs of an allergic reaction can include a number of factors, including any unusual swelling, excessive redness, shortness of breath or trouble with breathing. These should be addressed immediately. Since dentists may leave the treatment room after the injection, dental auxiliaries have a critical role in patient monitoring after the injection. Patients should not be left alone after local anesthesia has been administered. Patients of all ages should be observed to be sure they are not biting on anesthetized tissues. After a procedure is completed, auxiliaries should remind patients and caregivers to avoid biting or chewing to avoid tissue damage.
Recognizing and Managing Contraindications, Allergic Reactions, and Side Effects
About half of all emergencies in dental offices occur before or after administration of local anesthesia.5 Every dental team member should have and know the office protocol for managing emergencies, including who will call 911. Contraindications to local anesthetics are numerous. Before delivering local anesthesia, operators should always consult the product insert packaged with local anesthetics or the PDR. Each product has a maximum amount based on the patient’s weight. While most products are metabolized in the liver, plasma or both, the half life of the product is also important. This is the time that it takes to reduce potency by half. For 2% Lidocaine, this is about 90 minutes, and the half life for 4% Articaine is 30 minutes. Except for prilocaine, which is metabolized in the kidney and plasma, the amide linkage anesthetics are metabolized in the liver.7 Therefore, impairment in liver function is a key contraindication to local anesthesia. The half life of products should also be addressed, special consideration should be given to the duration of procedures and/or the age of the person, such as children under 12.
Allergies to local anesthetics can be confirmed by intradermal testing by an allergy specialist. Most allergic reactions are limited to the outer tissues and can be treated with antihistamines; the more serious ones require treatment with epinephrine.
The most common side effect of injections is syncope. Patients with a history of syncope should be considered for treatment with diphenhydramine.4 Allergic reactions to amide linkage anesthetics are relatively rare and mostly attributed to the preservatives or antioxidants found in the anesthetic. Ester linkage anesthetics have had a higher rate of reported allergy due to the para-aminobenzoic acid (PABA) preservative.
For documented allergy to both ester and amide groups, diphenhydramine can be used for procedures of short duration. A study that examined the impact of diphenhydramine administration in 17 patients found diphenhydramine efficacy similar to that found in seven patients using prilocaine. While larger studies are needed, diphenhydramine may be an effective alternative for patients with allergy to local anesthetics in emergency procedures.7 (See also 325 Malamed, Handbook of Local Anesthetics. Fifth Edition.)
Most reported allergic reactions are caused by the preservatives methylparaben and metabisulfite.8 Metabisulfite is added as an antioxidant when vasoconstrictors are used in anesthetics. For patients reporting a documented allergy to sulfites, avoid anesthetics containing vasoconstrictors. For such patients with documented sulfite allergies, plain anesthetics such as mepivacaine 3% or prilocaine 4% are available without the preservative.5
Latex allergies are commonly reported among patients. However, the latex stopper at the end of the cartridge is not made of “natural" latex commonly implicated in latex allergies. While the latex stoppers have not been implicated in available case reports of adverse reactions among dental patients, manufacturers of dental anesthetics must label any products that contain latex in cartridge anesthetics.9 As with many dental issues, no prospective epidemiologic study has evaluated this issue, but it cannot be ruled out in allergy situations. There are latex-free stoppers in certain brands of anesthetics available for patients with latex allergies. These are labeled as latex-free.
In addition to allergies, other contraindications are specific to certain anesthetics. Levonordefrin, an alternative to epinephrine, should not be used when a patient takes tricyclic antidepressants, and reduced dosages of epinephrine are recommended. For patients with significant cardiovascular disease, the dentist may choose to consult with their physicians. Recreational use of cocaine by patients can increase the risk of blood pressure and cardiac arrhythmias with injectable anesthetics.9-14 Data indicate that lidocaine and prilocaine may be safest for use among pregnant and lactating women.5 Paresthesia has been reported occasionally after local anesthesia with many of the amide linkages.11
ANATOMY
All operators delivering anesthesia must have a detailed knowledge of the regional anatomy to avoid unnecessary injury to the patient and potential legal action. Even the most experienced practitioner can benefit from periodic review of the anatomy associated with local anesthesia and injection protocols to minimize the risk of complications.15 Local anesthesia by block can be delivered to two of the three branches of the trigeminal nerve, the maxillary nerve, and the mandibular nerve. Lingual anesthesia is achieved in the mandibular regions, except for anterior teeth with a block. For maxillary teeth, lingual anesthesia may be obtained with local injection.
The Maxillary Nerve
The maxillary nerve has three divisions: the pterygopalatine nerve, the infraorbital nerve, and the zygomatic nerve.
The pterygopalatine nerve has several divisions, with two terminal branches that are most important in dental procedures. The anterior palatine nerve enters the oral cavity through the greater palatine foramen and is the larger of the two branches. It splits into a number of smaller branches at the greater palatine foramen and fans out as the greater palatine nerve, which supplies the mucosa of the hard palate to the canines. This nerve then goes into the palatine artery, which is inside connective tissue between the periosteum and the palatal mucosa. Injuries in the nerve endings in the palatal mucosa usually repair themselves, and patients will not normally experience any problems.
The posterior palatine nerve is the smaller of the two branches of the pterygopalatine nerve. This nerve, which provides sensory endings to the tonsils, goes through the lesser palatine foramen.
The infraorbital nerve encompasses three branches: the anterior, middle, and posterior superior alveolar nerves, which provide sensory endings to the maxillary teeth, the associated periodontal membranes, and gingiva on the lateral aspect of the maxilla. The nerve emerges at the infraorbital foramen. Injectable anesthetics act on the nerves in the superior dental plexus formed by the superior alveolar nerves in the base of the alveolar process. The patient will not experience any sensory deficits following procedures in this region.
Terminal branches of the infraorbital nerve fan out in the direction of the lower eyelid, nose, and upper lip from the infraorbital foramen. Several superior labial branches go into the lip between the muscles and mucous membrane to supply the mucosa of the upper lip and skin through the orbicularis muscle. When performing either apicoectomies on the maxillary canine or premolar teeth or carrying out sinus lift procedures on the atrophic maxilla, operators must be especially careful to avoid injuring this nerve where it arises from the infraorbital foramen. Such an injury can cause a traumatic neuroma with permanent neurological loss. Conversely, injuries to the terminal branches that end in the lip will repair themselves.
The zygomatic nerve is a branch of the maxillary nerve that divides into a facial branch supplying the skin of the prominent part of the cheek and a temporal branch supplying the skin of the anterior temporal region.
The Mandibular Nerve
Both motor and sensory fibers make up this mixed nerve, which has four sensory branches. Its internal branch includes two nerves, the buccal and lingual nerves, which supply large areas of the oral mucosa. The middle branch — inferior alveolar nerve — supplies the mandibular teeth, skin, and mucosal membrane of the lower lip and skin of the chin. The auriculotemporal nerve in the external branch is never anesthetized in dentistry.
The buccal nerve, which is not involved in dental procedures, may need to be anesthetized because it sometimes causes pain perception during retraction. This nerve proceeds along the most forward (anterior) portion of the temporalis muscle downward along and within the fascia, along the outer portion of the buccinator muscle. Multiple branches of the buccal nerve travel through the buccinator muscle, providing innervation for most of the mucosa of the cheek.
Sensory and taste fibers are found in the lingual nerve, which separates from the inferior alveolar nerve approxi-mately 5 to 10 mm below the base of the cranium. The lingual nerve is more forward (anterior) and slightly more to the middle (medial) in relationship to the inferior alveolar nerve. As shown in Figure 4, the lingual nerve follows along the outside (lateral) of the medial pterygoid muscle to the upper portion of the mylohyoid; at the mylohyoid muscle, the lingual nerve curves sharply forward (anteriorly) to continue on a flat plane across the inner surface of the floor of the mouth. This nerve is superficial in the back (posterior) portion of the oral cavity. It sometimes can be seen with the naked eye through the thin membranes of the lingual mucosa, beginning at the third molars to the second molars. The nerve turns medially near the first molar and goes under the submandibular duct, with multiple branches that innervate the tongue.
Removal of impacted third molars presents the highest potential for injuring the lingual nerve, as it is most exposed medial to the retromolar trigome. This is most likely to occur in patients who have had repeated episodes of pericoronitis. While Figure 4 shows the usual pattern of this nerve, not all patients have this pattern. In about 10 percent of patients, the lingual nerve is located at a higher level in relation to the internal oblique ridge. An injury in this location is likely to cause varying degrees of permanent damage. Microsurgical repairs have an 80 percent success rate for return to pain-free sensory function if they are done within 90 days of the injury.
The inferior alveolar nerve divides in the premolar region into the incisive and mental nerves, which supply the teeth and periodontal ligaments of the mandibular teeth. The mental nerve further divides into three to five branches after exiting the mandible through the mental foramen. The incisive branch stays within the mandible, where it continues and becomes part of the inferior dental plexus. The relative position of the lingual nerve varies depending on the age of the patient. As the mandible grows and moves more forward and more laterally, the lingual nerve becomes more posterior and superior to the ramus of the mandible. Beginning at the third molar area, the inferior alveolar nerve arches at the apex of the molars and continues below the roots of the first molars.
In the premolar region of the mouth, this nerve is about halfway between the roots and the lower mandible border. If dental surgery is planned in this area, the nerve should be located through the use of a panoramic image before the procedure begins. The inferior alveolar canal can be found about 4 to 7 mm from the mandible’s lateral cortical cortex. Third molar surgery presents the greatest risk of injury to this nerve but because the nerve is located inside the bony canal, nerve regeneration is more likely, along with the return of sensation, as long as fractured canal fragments do not block the canal. Microsurgical repair should not be considered until at least three months after the injury. Persistent neurosensory deficits are more likely in patients over age 40; in more than half of these patients, alveolar nerve injury may result in continuing problems, such as lip biting and drooling. For this reason, patients over age 40 should be given presurgical counseling on the possibility of such complications, and asymptomatic impacted third molars should not be removed.16
Relationship of Maxillary Nerve to Maxilla
Remember that the maxillary nerve branches into three different areas: one above and just posterior to the second molar, one branch just above the premolar, and one around the canine for the canine and lateral and central incisor. These are usual injection sites.
Relationship of Mandibular Nerve to Mandible
The mandibular nerve comes through the mandible just around the apex of the premolar or canine and exits. This is often the site of injection, and sometimes fibers from this nerve cross the midline, which can affect the profoundness of the anesthesia.
TECHNIQUES FOR DELIVERING ANESTHESIA
The dental assistant is often responsible for preparing the anesthetic syringe for use by the operator (i.e., the dentist or hygienist).
When assembling a syringe, always wear gloves and protective eyewear, keep the needle sterile, and use care to avoid needlesticks. Keep the needle pointed away from yourself at all times.
Needles are capped on two sides. Unlock the cap from the shortest side, holding the sharp end away from you. Screw this side of the needle into the hub of the syringe. Then, holding the syringe in one hand, insert an anesthetic cartridge into the syringe. At the same time use the other hand to pull back on the plunger, making room for the cartridge. Always keep the patient side of the needle capped and sterile at all times. The steps for assembling a syringe are summarized in Table 4.
Needles are available in long, short and extra short lengths. Short lengths are used for maxillary buccal injections or palatal injections and never for mandibular blocks. Extra short needles are used for periodontal ligament anesthesia. A long needle is used for mandibular blocks or for designated posterior maxillary injections, as specified by the dentist. Needles also come in different gauges. Needle gauge correlates with the diameter of the needle; the smaller the number, the greater the diameter of the needle. (International standard 9626, Amendment 1, Stainless steel needle tubing for the manufacturer of medical devices. 2001)
Many techniques may be used to minimize the discomfort and pain associated with the administration of anesthesia, some of which the dental assistant can perform. •Always explain the procedure to the patient in advance.
•Use relaxation techniques to ease the patient’s anxiety.
•Use vibrating devices, such as VibraJect® or DentalVibe®
Although its efficacy is still being studied, the VibraJect® is attached to the anesthetic syringe and when engaged causes the syringe and needle to vibrate. Pain is reduced through the Gate Control Theory. This theory is based on the fact that the vibration message is carried to the brain through insulated nerves and the pain message is carried through smaller uninsulated nerves. The insulated nerves overrule the smaller unisulated nerves. The vibration and hum of the motor may also have a calming effect. (Figure 10)
The DentalVibe® gently stimulates the sensory receptors at the injection site causing the neural pain gate to close which blocks the pain of injections. An advantage to this system is that the tissue is vibrated before the needle penetrates. A disadvantage is this is a separate unit and not attached directly to the syringe, so that both hands are engaged with this technique.26,27 (Figure 11)
Other techniques that operators can employ include:
Neutralizing the acidic properties of the anesthetic by using sodium bicarbonate, such as Onset®, as a buffering agent that reduces the burning sensation of the anesthetic. A buffering agent also reduces the time for anesthesia to become effective and is highly effective in situations where pH changes caused by local infection make profound anesthesia more difficult (see http:www.onpharma.com/MixingPen.html) The buffering agent is added to the anes-thetic cartridge before injecting. (Figure 12)
•Using pinching or pressure during the application to distract the patient. •Keeping the speed of the injection constant.
•Using vapo-coolants before the injection.
•Using a topical anesthetic at the site before the injection.
•Aspirating the syringe immediately after the needle is in injection site to check for blood.
Of all the techniques used to reduce pain, those found to be the most effective were slow, constant administration of the anesthesia.17 The use of warming the anesthetic may actually cause a breakdown of the epinephrine or levonordefrin. This breakdown makes vasoconstriction less effective, which results in shorter anesthetic times. This practice is not recommended.
OCCUPATIONAL SAFETY AND RELATED REGULATIONS AND RECOMMNEDATIONS
Avoiding needlesticks to the dental professional and patient is the biggest safety concern. Handling of the syringe post-injection, as well as during disassembly, are the two main times needlesticks occur. After the injection procedure the needle is contaminated with patient blood and fluid. Therefore, never pass an uncapped needle after a procedure and never point an uncapped needle toward the body.
Following injection, recapping of needles by hand is not recommended, as needlestick injuries can occur.
Use a recapping device for needles where possible. A variety of recapping devices are available; an example appears in Figure 13. If a recapping device is not available, the one-handed “scoop" technique is preferred for recapping needles between multiple injections on the same patient. The operator should not pass the syringe back to the assistant. Instead, the operator should recap the syringe. Precautions should be taken when disassembling the syringe, always wear heavy or neoprene gloves when cleaning instruments prior to sterilization processing. Disassemble the syringe with the needle recapped by pulling back on the plunger, removing the cartridge, and unscrewing the needle from the syringe hub. Do not bend or break needles during disposal. Dispose of the needle and cover in a sharps container. When a sharps container is full to its “fill" line, dispose of it according to state or local regulations for biohazardous waste. Dental needles are intended for single use only; they should never be reused.
Occupational Injuries, OSHA, and CDC
Since there is no active surveillance of dental offices for disease transmission nationally, healthcare associated infections (HAIs) to dental professionals as a result of needlestick and other sharps injuries in dental offices are not quantified. However, case reports and legal cases provide ample evidence that transmission of bloodborne infections does occur; therefore, prevention of sharps injuries is very important. Should an injury occur, the patient should be referred for evaluation for risk of disease and the injured personnel should be offered post-exposure prophylaxis after consultation with an infectious disease expert within the local health department or hospital facility. Your local contact should be listed in the sharps injuries protocol in your office.
The Centers for Disease Control and Prevention (CDC) estimate that approximately 600,000 to 1,000,000 needlestick and other percutaneous injuries occurred annually among U.S. healthcare workers, potentially exposing medical and dental team members to bloodborne pathogens such as human immunodeficiency virus (HIV), hepatitis B virus (HBV), and hepatitis C virus (HCV). Numerous studies have demonstrated that as part of an overall safety and injury-reduction program, the use of safer medical devices, such as needleless systems and sharps with engineered safety features can be extremely effective in reducing accidental sharps injuries. According to CDC, 62 to 88 percent of sharps injuries potentially could be prevented through the use of such devices.(Figure 14)
Although the 1991 federal Occupational Safety and Health Administration (OSHA) Bloodborne Pathogens Standard (29 CFR 1910.1030) required the use of engineering controls to help decrease the risk of occupational sharps injuries in health-care settings, the Needlestick Safety and Prevention Act adopted by Congress in 2000 called for expansion of the OSHA standard.18 The resulting 2001 revision of the Bloodborne Pathogens Standard specifically requires the review and consideration of “sharps with engineered sharps injury protections." For dental applications, such devices include safety needles and/or safety syringes that may be used to deliver local anesthesia. (Figure 15A and 15B) Since the law went into effect in 2001, the number of reported needlestick injuries has decreased by one-third.23
The revised OSHA standard now requires:
•annual consideration and implementation of appropriate engineering controls, including needleless systems and/or sharps with engineered sharps injury protections;
•inclusion of non-managerial healthcare workers in evaluating and choosing devices; and
•documentation of these efforts within the practice setting’s OSHA-required exposure control plan.
To comply, at least annually the employer must:
•review newly available devices designed to reduce sharps injuries;
•document consideration of sharps with engineered safety features as well as use of appropriate, commercially available, effective safer devices; and
•document employee involvement in the device review evaluation process.
Because OSHA recognizes that no one medical device can be considered appropriate or effective for all circumstances, it defines an “appropriate" safer medical device as one whose use, “based on reasonable judgment in individual cases, will not jeopardize patient or employee safety or be medically contraindicated." OSHA defines an “effective" safer medical device as one that, based on reasonable judgment, will make an exposure incident involving a contaminated sharp less likely to occur. To help determine if available safer sharps devices are appropriate and effective in the individual practice setting, CDC has created a set of sample Screening and Evaluation Forms, with an introduction that explains the process of safely evaluating new sharps safety devices for the individual practice setting. The forms and introduction are available through the CDC website: http://www.cdc.gov/oralhealth/infectioncontrol/forms.htm
Postexposure Management
Even with engineering controls in place, accidents can happen. Needlesticks and other occupational sharps injuries are considered medical emergencies and must be evaluated promptly by a qualified heath-care provider to best decrease the risk of transmission of infection with HBV, HCV, HIV or other bloodborne pathogens. In the current “Guidelines for Infection Control in Dental Health-Care Settings, 2003,"19 CDC provides detailed information on postexposure management. The complete document, which also includes information on sharps safety and engineering controls, is available at the CDC website: "http://www.cdc.gov/OralHealth/infectioncontrol/guidelines/index.htm
The Needlestick Safety and Prevention Act also calls for health-care facilities to maintain a sharps injury log. Although dental offices are classified by OSHA as a low-injury industry and thus exempt from this requirement, practices can benefit from this type of recordkeeping. A sharps injury log can provide valuable information on the products and work practices within the dental setting that are most commonly implicated in occupational injuries. In turn, such information may be used to develop interventions that reduce or eliminate those risks within the practice setting.
Appendix I reproduces OSHA’s Form 301: Injury and Illness Incident Report, which can be used to record the circumstances of sharps injuries within the practice. The form is also available via the OSHA website: "https://www.osha.gov/recordkeeping/new-osha300form1-1-04.pdf.
A comprehensive sharps injury log must include detailed information on the percutaneous injuries sustained in the practice setting, including:
•the type and brand of device involved in exposure incidents,
•the department in which the exposure occurred, and
•an explanation of how the injury occurred.
For more information on preventing and documenting sharps injuries in the dental practice, visit the Organization for Safety and Asepsis Procedures’ (OSAP) website at www. osap.org/?Issues?SharpsSafety and for OSHA issues go to www.osap.org/?page=GuideOSHA.
States that have their own OSHA plans are required to have regulations that are “at least as effective" as those prescribed by the federal OSHA regulations. As such, dental practices operating in areas with state-run OSHA plans should ensure that they are in full compliance with the rules for their state. In addition, many states require that newly introduced engineering controls for injection equipment be reviewed by the state. Check your state OSHA requirements, as state OSHA requirements vary.
MANAGING EMERGENCIES
Emergencies, including life-threatening events, can happen to anyone at any time, but the stress associated with dental procedures can increase the risk that they may occur. About half of all emergencies occur around the time of injection, so be prepared with a written protocol. In addition to the steps that dentists can take while administering anesthetics, the dental assistant can help prevent some emergencies by always following certain procedures:20
•Never underestimate the importance of the medical history. Always obtain complete information about any change in health status or drugs at the preoperative appointment and update it at the beginning of each appointment.
•Before the local anesthetic is administered, address any fears or nervousness the patient may be experiencing.
•Make sure the patient is in a supine position for the injections.
•Watch patients throughout the administration of anesthetics. Do not leave them alone following the injection.21
To be prepared for any contingencies, dental offices must not only have a plan for managing emergencies, but also review the written plan on a regular basis. The plan should include procedures for addressing events such as patient unconsciousness, breathing problems, seizures, drug-related reactions, or chest pain. The most important part is to know who will call 9-1-1 in the case of any life-threatening emergency. Life-threatening emergencies include a patient having difficulty breathing, chest pains or difficulty swallowing and/or immediate facial swelling or redness.
Plans should exist in writing and should detail the roles of each staff member in case of an emergency. Different offices have different capacities for managing emergencies, from minimal to full resuscitation procedures. All dental assistants should know how their offices manage medical emergencies. Report any unusual occurrence or destabilization of the patient to the dentist immediately. In case of a medical emergency, know who in the office is responsible for calling 9-1-1 immediately.
•In an emergency, ensure that someone remains with the patient at all times, monitoring breathing and heart rate until the emergency is past or emergency medical personnel arrive.
•Be prepared to assist with cardiopulmonary resuscitation (CPR). The American Heart Association and the American Red Cross provide basic life support classes, and many states require dental health-care workers to complete these courses. Be familiar with the procedures used in the office.
•Know the location of the emergency kit or equipment as well as the staff members who have access to it. Because of the kinds of medication it contains, these kits are often locked so be sure to know where to locate the key.
Emergency procedures should be explained to new employees on their first day on the job. The entire staff should practice staged emergencies at least semiannually; medical-emergency training records should be kept along with the OSHA-required training records.
The office emergency kit should include the drugs and equipment necessary for addressing a wide range of emergencies. Emergency oxygen should be available as well. Everyone in the practice setting should know how to access this kit or equipment and how to correctly use it.
Allergic reactions are among the most common life threatening emergency in the dental setting and must be addressed promptly. Specific plans should be in place for managing allergies to local anesthetics in patients and should be regularly reviewed with the entire treatment team. While allergic reactions are rare, they can occur.21 A speedy response, including calls to 9-1-1 by a designated staff member, should be part of the plan. Response plans should be reviewed quarterly and in annual OSHA training to assure a prompt response to any potentially life-threatening allergic reactions.
NEW TECHNOLOGIES
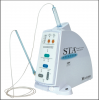
Although Cook invented the modern dental syringe more than one hundred years ago, it is only recently that anesthetic delivery systems have seen major innovations. One new device, the STA or Single Tooth Application Wand™ (Figure 16), uses a microprocessor to control the delivery of a small amount of anesthesia ahead of the needle, thus ensuring a steady flow of anesthetic through the needle into the tissue. According to the manufacturer, this delivery method reduces the amount of pain that patients experience and increases their comfort. In addition, delivering anesthesia using this device may help patients avoid numbness of the tongue, lips, face, and other muscles.
In response to the Needlestick Safety and Prevention Act, delivery devices, such as the STA and The Wand ™ (Figure 17) have been developed (http://www.stais4us.com) with engineering controls for anesthesia delivery. The safety system has a pen-like grasp that allows maximum tactile control and an auto-retracting design that shields the needle when not in use. The rate of injection is at a preprogrammed technique-specific rate selected by the dentist. A disposable cartridge sheath is required for each patient, but a standard dental needle and anesthetic cartridge can be used with this device. There are likely to be more delivery syringes available in the near future.
As with any medical device, follow the manufacturer’s instructions for use, and apply the same safety principles as when handling any other sharp device. In addition, a nasal spray mist will soon be available for use to anesthetize maxillary teeth that will not use a needle. The tip is inserted and sprayed into the nasal cavity (see http://st-renatus.com/)
LOCAL ANESTHESIA REVERSAL AGENT
The most annoying side effect of local anesthesia with vasoconstrictor is the lingering numbness of the soft tissue associated with minor dental procedures. This numbness may cause drooling, a crooked smile, diminished ability to speak properly, and injuries from unknowingly biting the lips, cheeks, and/or tongue. Among children, post-anesthetic trauma can occur when they chew the lip or tongue. This has the potential to be serious for young children. In addition, busy patients must often return to work or school without residual numbness.
Phentolamine Mesylate, sold under the brand name of OraVerse®, is an anesthetic reversal agent that reduces time of numbness by half. It is injected using the same technique that is used in local anesthesia, with about half the dosage of anesthetic used. Although not covered yet by insurance, it is becoming a standard of care in many practices. It is not indicated in children under 6 years of age or persons weighing less than 33 lbs.24,25
SUMMARY
The success of the contemporary dental practice largely hinges on the use of local anesthesia for ensuring patient comfort and safety. Dental professionals should be aware of proper methods for handling syringes and needles, avoiding needlestick and sharps injuries in the office, complications of anesthesia, and how to manage any emergencies.
A periodic review of anesthesia techniques is important for keeping abreast of recent developments in dental pain control. The review should include an introduction to new anesthetics, innovations in anesthesia or delivery devices as well as a discussion of complications of local anesthetics and their administration.
Infection control and sterility should be maintained during all anesthetic procedures. Should a needlestick occur, manage the exposure immediately according to OSHA regulations and CDC recommendations.
REFERENCES
1. Reed KL. A Brief History of Anesthesiology in Dentistry. Texas Dent J 2002 Mar; 219-224.
2. ADA House of Delegates. Guidelines for Teaching the Comprehensive Control of Pain and Anxiety in Dentistry. 2007. www.ada.org/sections/about/pdfs/anxiety_guidelines.pdf. Accessed January 22, 2014
3. Scarlett MI. Current Concepts in Local Anesthetics. Woman Dent J. 2004 Apr; 32-38
4. Meechan JG. Effective Topical Anesthetic Agents and Techniques. Dent Clin North Am 2002 Oct;46(4):759-66.
5. Malamed, SF, Reed, KL, and Fonner AM. Local Anesthesia Part 2: Technical Considerations. Anesth Prog. 2012 Fall; 59(3): 127–137. doi: 10.2344/0003-3006-59.3.127 PMCID: PMC3468291
6. www.oraqix.com/properties.aspx and www.oraqix.com/safety.aspx. Accessed January 22, 2014
7. Uckan S, Guler N, Sumer M, Ungor M. Local Anesthetic Efficacy for Oral Surgery: Comparison of Diphenhydramine and Prilocaine. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998 Jul;86(1):26-30.
8. Haas DA. Localized Complications From Local Anesthesia. J Calif Dent 1998;26: 677-682.
9. Shojaei AR, Haas DA. Local Anesthetic Cartridges and Latex Allergy: a Literature Review. J Can Dent Assoc 2002 Nov; 68(10):622-6.
10. Eggleston ST, Lush LW. Understanding Allergic Reactions to Local Anesthetics. Ann Pharmacother 1996 Jul-Aug;30(7-8):851-7.
11. Haas DA, Lennon D. A 21-year Retrospective Study of Reports of Paresthesia Following Local Anesthetic Administration. J Can Dent Assoc 1995:61:319-330.
12. Haas DA. Localized Complications from Local Anesthesia. J Calif Dent 1998; 26: 677-682.
13. Finder RL, Moore PA. Adverse Drug Reactions to Local Anesthesia. Dent Clin North Am 2002 Oct;46(4):747-57.
14. Blanton PL, Jeske AH. Dental Local Anesthetics: Alternative Delivery Methods. JADA 2003 Feb;134(2):228-34.
15. Blanton PL, Jeske AH, ADA Council on Scientific Affairs, ADA Division of Science. Avoiding Complications in Local Anesthesia Induction: Anatomical Considerations. JADA 2003 Jun;134(6):753-60.
16. Kaweckyj N. Maxillofacial Surgery Basics for the Dental Assistant. Part I. American Dental Assistants Association 2014.
17. Meit S, et al. Techniques for Reducing Anesthetic Injection Pain—An Interdisciplinary Survey of Knowledge and Knowledge and Application. JADA 2004 Sep;135:1241-1250.
18. U.S. Congress. The Needlestick Safety and Prevention Act (HR 5178). Available at http://www.osha.gov/SLTC/etools/hospital/hazards/sharps/sharps.html. Accessed January 22, 2014.
19. 19.CDC. Guidelines for Infection Control in Dental Health-Care Settings-2003. MMWR Morbid Mortal Weekly Report December 19, 2003;52 (RR17);1-61.
20. Protzman S, Clark J. The Dental Assistant’s Management of Medical Emergencies. American Dental Assistants Association 2011.
21. Blanton PL, Jeske AH. Misconceptions Involving Dental Local Anesthesia. Texas Dent J 2002; 119(4): 296-307.
22. Milestone Scientific. Available at http://milestonescientific.com/dental.html. Accessed April 20, 2014.
23. Phillips EK, et al. Issues in Understanding the Impact of the Needlestick Safety and Prevention Act on Hospital Sharps Injuries. Infection Control and Hospital Epidemiology: Sept 2013.
24. Tavares M, et al. Reversal of Soft-Tissue Local Anesthesia with Phentolamine Mesylate in Pediatric Patients. JADA 2008 Aug; 139, 1095-1104
25. Hersh EV, et al. Reversal of Soft-Tissue Local Anesthesia with Phentolamine Mesylate in Adolescents and Adults. JADA 2008 Aug; 139, 1080-1093
26. Hirst, L. Good Vibrations? – DentalVibe vs. Vibraject. Dental Anxiety Network: December 9, 2013. http://www/dentalanxiety.net/gadgets/dentalvibe-vs-vibrajet. Accessed May, 1, 2014.
27. Saijo, M, et al. Lack of Pain Reduction by a Vibrating Local Anesthetic Attachment: A Pilot Study. Anesthesia Progress. American Dental Society of Anesthesiology: Summer 2005: 52(2): 62-64. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2527045. Accessed May 1, 2014.
ABOUT THE AUTHOR
Margaret I. Scarlett, DMD
Margaret I. Scarlett, DMD, is an accomplished clinician, scientist, and lecturer who retired from the Centers for Disease Control and Prevention after 23 years of federal service. She is a past author and editor of several dental publications, and a past president of the American Association of Women Dentists. As an innovator, including writing the very first 1986 CDC infection control guidelines for dental health-care workers, she continues to explore new and better ways to deliver prevention, care and treatment of the oral cavity. She consults on intraoral health and primary care and is a leading dental expert in infectious and chronic diseases and systemic-oral health issues.